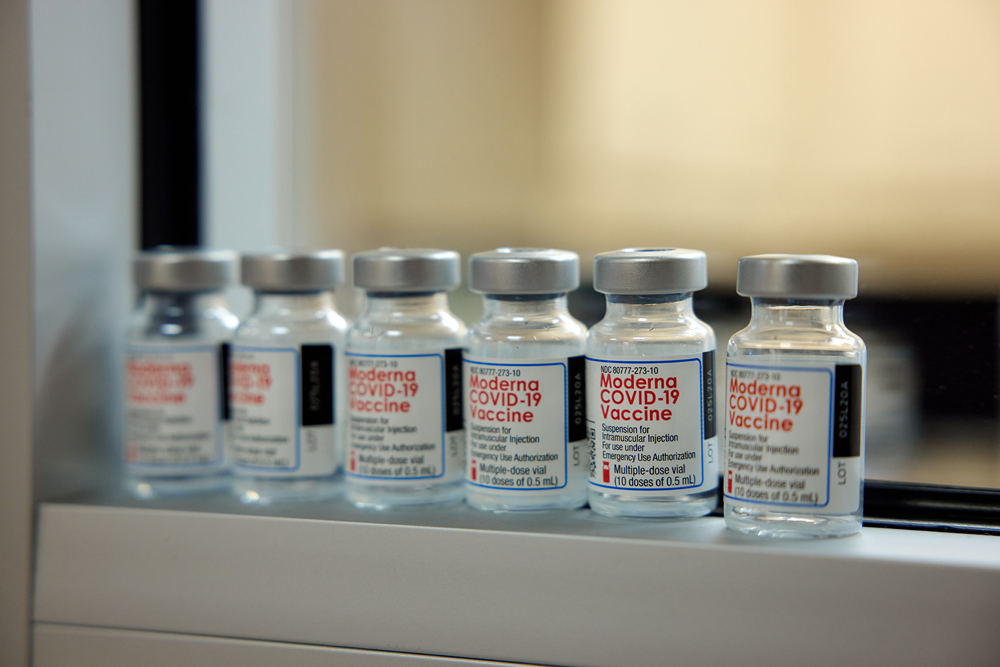
Photo by Andrew Emery
Closing the Covid Vaccination Gap
Jackie Zhuang’s research points to strategies to overcome Black Americans’ hesitancy.
Throughout the Covid-19 pandemic, Jie “Jackie” Zhuang has been puzzled about why so many Black Americans appear reluctant to get vaccinated even though they have been disproportionally impacted by the virus.
“I need to make sense of what I see on TV every day, hear on the news and see in people around me,” said Zhuang, an assistant professor of communication studies at TCU. “The vaccine is an effective tool and has been made widely available to the public. So, what is the problem? What’s missing in health communication?”
The answers, she said, lie in delivering the right messages through the right messengers to persuade a population inclined to mistrust the health care system.
While Black Americans face about the same odds of getting Covid-19 as white people, they’re roughly three times as likely to be hospitalized and twice as likely to die, according to the U.S. Centers for Disease Control and Prevention. And as more transmissible variants such as delta and omicron have surged, hospitalizations and deaths have risen mainly among unvaccinated people.
Low vaccination rates hurt efforts to achieve broad protection nationwide and exacerbate racial health disparities and the virus’s greater impact on people of color.
Preliminary results of Zhuang’s study show Black adults perceive a low prevalence and low social acceptance of Covid-19 vaccinations in their immediate social circles and among all Black Americans. But perhaps the biggest surprise, she said, were indications they were more likely to get vaccinated if their family doctors supported it.

Jie Zhuang, assistant professor of communication studies, is researching the acceptance of the Covid vaccine in the Black community. Photo by Rodger Mallison
“We focus a lot on media reports and CDC alerts, but I think we probably unintentionally neglected the role played by family doctors,” she said. “While it’s important to have a large-scale, message-based intervention, our health care providers need tools to initiate a conversation with their patients.”
A Legacy of Mistreatment
Many Black Americans have long mistrusted the health care system because of past medical racism, as illustrated by the case of Henrietta Lacks and the Tuskegee experiment, in which the U.S. government studied syphilis among 600 Black men from 1932 to 1972 without telling them of their illness or treating them for it. In the Lacks case, doctors took cells from her without her consent shortly before she died of cervical cancer in 1951. Lacks’ cells have been bought and sold to use in medical research.
While history cannot be ignored, more recent incidents and personal experience may be larger factors in explaining current medical skepticism and vaccine hesitancy. In a 2020 Facebook video that went viral, Dr. Susan Moore of Indiana accused her doctors of withholding Covid-19 treatment and pain medication because she was Black. “I put forward and I maintain, if I was white, I wouldn’t have to go through that,” she said in the video. Moore died later that year.
As of mid-July 2022, 10.1 percent of Black adults were fully vaccinated against Covid-19 and 10.3 percent had received at least one dose, according to CDC data.
Getting the Message Across
For her study, Zhuang surveyed the same group of unvaccinated Black adults nationwide three times in 2021. The first survey in early June included over 1,200 people, the second was roughly 400 people in early July, and the third included about 260 people in late July. She received a TCU Invests in Scholarship grant of $20,000 to help fund the research.
Collecting data from the same group of people over multiple points in time “will always provide more and better information than a one-time, cross-sectional survey,” said Paul Schrodt, the Philip J. & Cheryl C. Burguières Professor of Communication Studies at TCU and Zhuang’s mentor. “The thing that has impressed me the most about Jackie’s research is her thoughtfulness, precision and care of how she thinks through all aspects of research and design.”
Zhuang’s research found that changing people’s perception of social acceptance may affect their behavior, but who delivers health messages and what the messages are can be crucial.
Personalizing easy-to-understand information may be more effective than supplying blanket information or comparing them to other racial/ethnic groups, she said.
Karen Lincoln, founder of Advocates for African American Elders and an associate professor of social work at the University of Southern California, agreed.
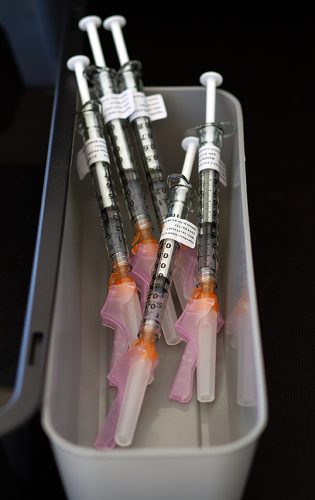
Covid-19 vaccines waiting to be administered during a drive-through vaccine clinic held at TCU. Photo by Mark Graham
“It’s very important to tailor health messages to certain groups based on culture, ethnicity, race, language and literacy levels,” Lincoln said. “We need to focus more on crafting the message and who the messenger is.”
Useful Information
Mary Bresnahan, a professor emeritus in Michigan State University’s department of communication who advised Zhuang on her master’s and doctoral degrees, said Zhuang is on track to be a leading health communications scholar.
“She commands a range of analytical skills and a deep understanding of statistics” to interpret large pools of data, said Bresnahan, who has collaborated often on research with Zhuang. “No stone goes unturned when working with Jackie. In scholarly research, that’s a good thing.”
Zhuang said she hopes to expand her Covid-19 research to a larger database or further explore the doctor-patient relationship.
In other research, Zhuang tends to tackle practical topics that are useful to the public, not just other academics, such as misperceptions of how HIV spread in her native China, Michigan residents’ perceived risks of dioxin pollution, stigmas toward veganism and various aspects of breastfeeding.
“I don’t want my research to stay in the journal,” she said. “As a health communications scholar, I’m not as interested in changing people’s attitudes as changing their behavior.”

Your comments are welcome
Comments
Related reading:
A Weapon Against Covid
An existing anti-rejection drug could combat life-threatening inflammation in Covid patients.
Alumni, Features
The Methodical Leader: How Barclay Berdan ’76 Built a Health Care Legacy
From Ebola to a global pandemic, the Texas Health Resources CEO built a reputation on listening first and deciding well.
Research + Discovery
Brandon Manning Examines Black Masculinity
His book Played Out: The Race Man in 21st Century Satire is an examination of inclusion and social justice.