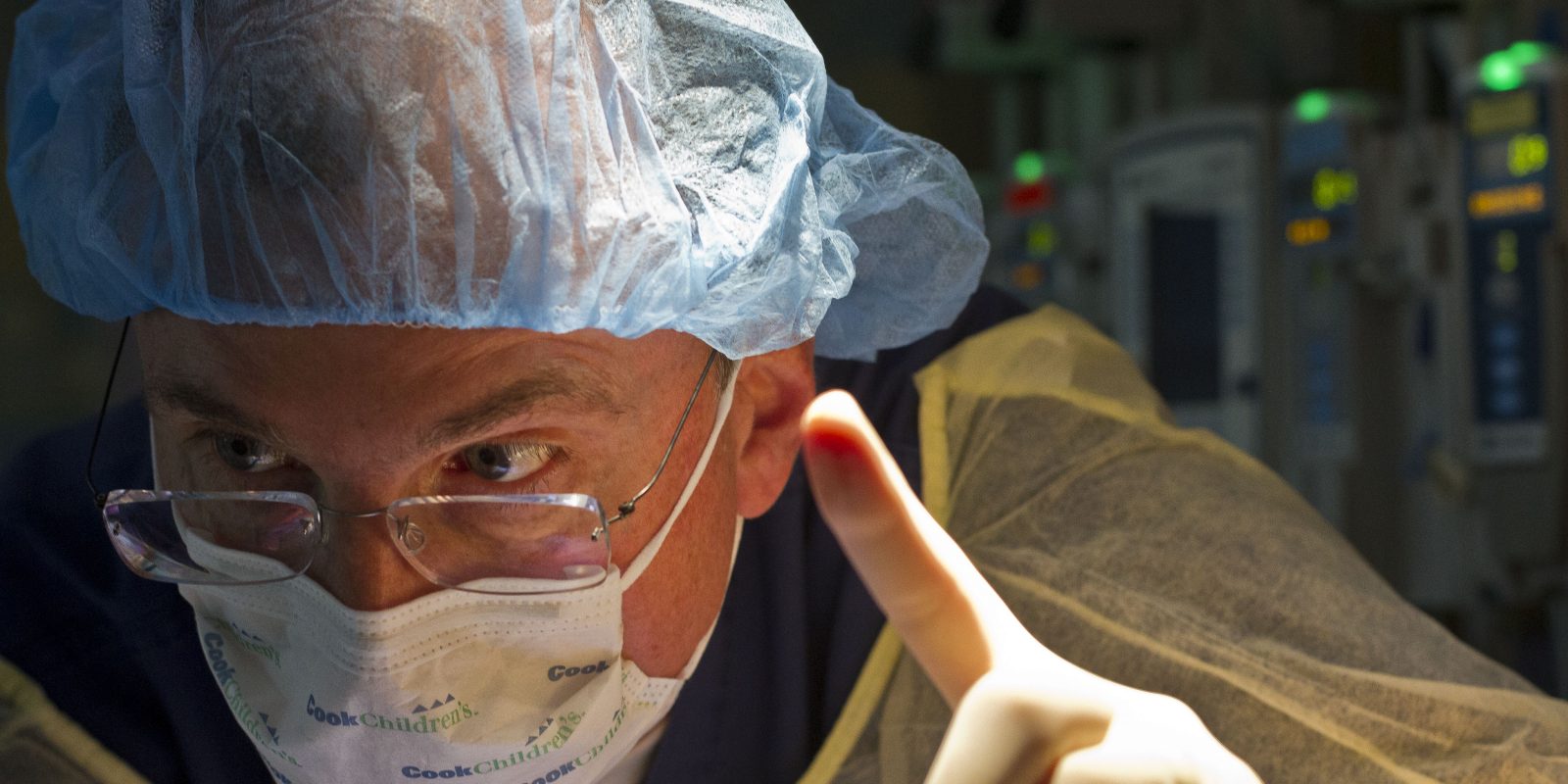
Dr. Jim Marshall performs a medical procedure on an infant at Cook Children's Health Care System in Fort Worth.
TCU Partnerships Shape the Future of Medicine
Leadership programs at two Fort Worth hospitals take physicians into uncharted territory.
Peaks the Dragon sat among dozens of furry friends inside a Build-A-Bear Workshop. The mythical blue and lime green creature is the mascot of Cook Children’s Health Care System in Fort Worth.
A 4-year-old boy and his 2-year-old sister went through their bears’ heart ceremony, dancing with and kissing the small fabric hearts when instructed. The children closed their eyes and made wishes before inserting the hearts into the cotton stuffing.
The boy, missing a couple of front teeth, selected an outfit while a Build-A-Bear employee sewed up his black bear. The boy’s outfit, red Chuck Taylors, jeans and green MVP T-shirt, was complete with a badge of honor: a Thomas the Tank Engine sticker. He chose a blue outfit for his bear and a hat with ear holes for good measure.
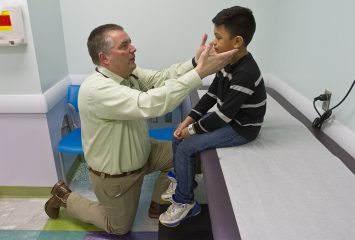
Dr. Donald Beam, medical director of the Life After Cancer Program at Cook Children’s Health Care System, examines Malachi Ordonez. Photo by Mark Graham
Once upon a time, Dr. Donald Beam, medical director of the Life After Cancer Program at Cook Children’s, and his fellow physicians thought amenities such as Build-A-Bear (the first of its kind in a hospital) distracted patients, making them late for their appointments.
Physicians often are aware of such operational issues but don’t always have a seat at the table when hospital administrators make choices. That may be changing, however, since Cook Children’s and another hospital in Fort Worth teamed up with TCU Neeley Executive Education to equip health care professionals with leadership and business tools.
Working with the executive program, hospital administrators customized course curriculums and project assignments for their organizations’ emerging leaders in the business of health care.
In the Cook Children’s leadership program, Advancing Healthcare Leadership, Beam’s project team members realized they were wrong about the reason for patients’ appointment delays. The misperception was uncovered when the group was tasked with improving the throughput, or the time from patient arrival to departure.
A digital time stamp showed the hospital’s fun features, such as Build-A-Bear, the tongue drum in the Child Life Zone or the hospital’s Lego model, did not cause the delays. Walking through the hospital’s throughput steps, the physicians in Beam’s leadership group witnessed superfluous procedures instead of the straightforward process they expected.
For example, the inpatient medical records system required patients’ parents to redo and re-sign forms during every visit. The group’s suggestion: minimize redundant paperwork. With a combination inpatient/outpatient system, all visits would be linked.
“The goal is to not just improve the patient experience, but I think if people get through this process and they’re not as stressed and not as frustrated, they get much more out of it,” said Beam, a pediatric hematologist/oncologist. “It’s a 100 percent reflection of us. The happy patient is the one who is more likely to do the right thing.”
I think that when you see you can make even a small impact on people’s lives, then that behooves you: Maybe I can make a big impact.
Dr. Donald Beam, medical director of the Life After Cancer Program at Cook Children's
Another delay stemmed from the hospital’s front desk. Rather than seeing patients on a first-come, first-served basis, as the leadership group assumed was the procedure, the front desk’s staff shuffled charts based on whether they thought a particular medical assistant would be better at drawing blood. “That was putting a lot of chaos into the way patients were being seen,” Beam said.
A discussion with medical assistants led to a conversation with the front desk staff and a resolution. Wait time decreased five minutes. Multiply that by 40 patients a day for one physician, and it’s a real time-saver.
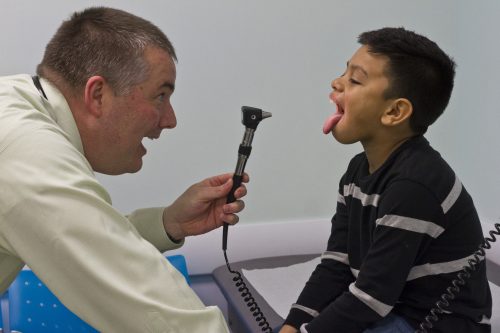
Dr. Donald Beam examines Malachi Ordonez. The physician’s leadership group analyzed Cook Children’s throughput process. Photo by Mark Graham
“When you’re a physician, a lot of times you can feel like a cog in the great big machine. This course lets you look as a leader: What can I do to make change?” Beam said. “It feels great that you can make an impact. I think that when you see you can make even a small impact on people’s lives, then that behooves you: Maybe I can make a big impact.”
Beam, like many of the physicians participating in the Cook Children’s leadership program, was unsure of what to expect when he started Saturday sessions at the business school. “I had no idea,” he said. “I mean that’s how foreign this is. You don’t know if you are going to be doing trust falls — you don’t know exactly what is going on.”
Molding Physician-Leaders
A few years ago, hospital administrators at Cook Children’s were searching for a leadership program for their physicians. They turned to the management experts at TCU’s business school.

Dr. Britt Nelson, president of Cook Children’s Physician Network, said he wanted a leadership program that would teach physicians skills they didn’t learn in medical school. Photo by Mark Graham
“In most places around the country, a physician becomes a doctor and they go to work and that’s it,” said Dr. Britt Nelson, president of Cook Children’s Physician Network. “There’s this sudden void in our lives because you’ve always been able to raise your hand and ask a question. You’ve always been at the top of your class. You’ve always had something next.”
Nelson and Robert Goodwill, senior vice president and chief operating officer at Cook Children’s, compiled a list of physician leadership organizations across the country and Dallas-Fort Worth universities with business schools and leadership programs.
“We went through a vetting process,” Nelson said. “TCU won pretty much hands down. They offered excitement. I think it’s a great marriage as far as the desires both institutions have.”
Cook Children’s started its first leadership cohort in August 2015 with 26 physicians. For the hospital’s second cohort of participants, the program added hospital administrators. The third cohort, which ends in April 2018, has 28 physicians, administrators and nurses.
Hospital administrators select the leadership program participants and assign their final projects, such as the one tackled by Beam’s group.
If you’re going to be a leader, you have to lead a ton of stuff you have no clue about. You may not even be interested in it, but you’ve got to get it done.
Dr. Britt Nelson, president of Cook Children's Physician Network
“The things in our organization go at a snail’s pace if there’s not some physician who has caught the vision, and even then it’s slow,” Nelson said. “Without the physician input, it won’t go anywhere.”
To really turn things on their heads, Nelson said, leadership participants were assigned projects in which they didn’t have any expertise in the topic. The strategy was met with some complaints, confusion and questions such as, “I don’t have anything to do with this — why am I on this?”
“That’s exactly the point,” Nelson said. “If you’re going to be a leader, you have to lead a ton of stuff you have no clue about. You may not even be interested in it, but you’ve got to get it done.
“There’s also a little bit of ‘you don’t know what you need,’ ” Nelson said. “It’s a completely different mindset from what you’re taught from kindergarten to medical school through the end of your residency — you don’t get a lot of this.”
Projects Solve Problems
Just as Cook Children’s administrators concluded that TCU’s business school could resolve its vacuum in health care leadership training, staff administrators at the John Peter Smith Health Network in Fort Worth came to the same decision.
JPS started its first Physician Leadership Program cohort in 2017. Hospital administrators selected the first group of physicians. Those inaugural participants then recommended the next cohort. But small groups in each JPS cohort selected their own projects.

Dr. Jo Anna Leuck checks on a patient in the emergency room at John Peter Smith Hospital. Leuck, who has a big hand in training emergency physicians, worked on a better orientation process for physicians with her group. Photo by Mark Graham
Dr. Jo Anna Leuck ’00, vice chair of academics for the department of emergency medicine and the department director for the emergency medicine residency program at JPS, spent two years working on an orientation process for new physicians. She asked her leadership group to take on the project.
“I have not been able to single-handedly make it happen,” Leuck said. “Then I went through this [leadership] course. Through the design thinking [class] and really considering the end user and how it would affect them, and having the team behind me, our small group really led to us being able to have orientation starting in August [2017].”
Dr. Anthony Zepeda, a hospitalist and family physician at JPS, was part of Leuck’s project group. He said the team developed an orientation that hopefully helps new physicians learn how the hospital’s system works so they will feel like part of the JPS family.

Dr. Anthony Zepeda smiles while checking on Tommy Schindler at John Peter Smith Hospital. Zepeda’s team worked on an orientation session for physicians at JPS. Photo by Mark Graham
“Most of us were trying to ask how we could bring other people to be as excited about working here at JPS and as excited about medicine in general,” Zepeda said.
In addition to solving the orientation obstacle, Leuck applied course sessions to her everyday life. “It’s hard to think about what I’ve not used,” she said. The main course that resonated with her was “Negotiation Skills for Physician Leaders,” learning that everything in life is about negotiation, from changing lanes with her car to stressful patient-care situations at the hospital.
For Zepeda, who hadn’t been in the classroom for more than a decade, an applicable course was “Motivating and Managing People” with Mary Uhl-Bien, BNSF Endowed Professor of Leadership at TCU. He said his leadership cohort learned how to motivate people who were on the outskirts of a team and not as enthusiastic about working in the group.
“[Uhl-Bien] took a lot of those topics in the beginning and asked us what we would want to learn,” Zepeda said. “I feel like the program kind of modified as time went on. She started to take some of those questions and bring them back and help us out with that. I think all of those questions became immediately applicable to us as [doctors] here.”
I was able to learn a new language on how to interact with the business side of medicine.
Dr. Anthony Zepeda, hospitalist and family physician at JPS
Zepeda said the professional conferences he attended over the years did not provide the problem-solving skills he needed for issues he encountered at work. For example, he became the leader of a committee at JPS, which was a new professional experience. “I didn’t feel like I had all the tools for that. I think being thrown into the cohort helped out a lot. I was able to learn a new language on how to interact with the business side of medicine.”

Dr. Jo Anna Leuck treats a patient in the emergency department at John Peter Smith Hospital. Photo by Mark Graham
Leuck said her leadership cohort had time to debrief and discuss what comes next. “I said to the group, ‘I’d be so disappointed if this was just a glorified kumbaya talking about how great this class was and then we walk away and nothing’s changed,’ ” she said. “So what we’re committed to, as the original 15 in the first cohort, is to partner with the next class and serve kind of as mentors for them on their group projects.
“That’s why I think it’s going to be really important to network and just to watch this grow,” Leuck said. “That’s how you change culture — you build networks.”

Dr. Jocelyn Zee, right, goes over a procedure with medical students Rubin Varghese, left, and Theron Bauman at John Peter Smith Hospital in Fort Worth. Photo by Mark Graham
Improving Communication
A nurse in periwinkle scrubs asked a health care peer about a doctor’s whereabouts as she twirled a bottle of hand sanitizer on the counter of the nurse’s station.

Dr. Jocelyn Zee goes over a procedure with Dr. Kevin Melgren, left, and medical student Theron Bauman at JPS. Photo by Mark Graham
“Ultimately, if you can’t get ahold of your fellow attending physician about a certain issue, then your care of your patient either gets delayed or you don’t really know who is taking care of your patient,” said Dr. Jocelyn Zee, an intensive care unit physician at JPS. “There seemed to be frustration that we were trying to measure.”
Zee’s project group identified areas of communication that were lacking among physicians. Members started with a survey and discovered a problem across the institution. Not everyone had a work cellphone, and as for pagers, physicians questioned if they had the right number for the appropriate medical peer.
To combat these communication concerns, Zee’s project group developed “PhysID,” a secure online directory only accessible to attending physicians who register for it. This means JPS administrators, including CEO Robert Earley, are not granted access.
“We had Mr. Earley try to log in and it said, ‘We’re sorry. We’re glad you’re our CEO, but you don’t have access to our physician directory,’ ” Zee said. “He was totally cool with it. He was really fine about knowing that physicians want to be able to talk to each other [and] feel like it’s a safe, productive environment.”
Putting the Pieces Together
Physicians at Cook Children’s brought varying sums of experience and levels of expectations to the hospital’s customized leadership program at TCU.
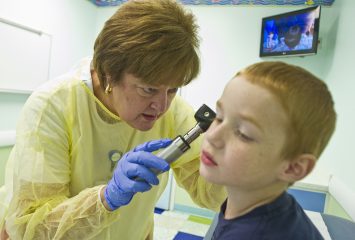
Dr. Nancy Dambro, pediatric pulmonologist, examines Jaiden Higginbotham at Cook Children’s Hospital. She found the tailored leadership program’s business orientation useful in her interactions. Photo by Mark Graham
Dr. Nancy Dambro, a practicing physician of pediatric pulmonology at Cook Children’s, has more than 30 years under her stethoscope. She also has served on numerous committees, held a medical directorship and has taken quality improvement courses throughout her long career.
Dambro, chair of Cook Children’s risk management committee, said the tailored leadership program’s business orientation was a good idea, rather than just focusing on hospital quality and leadership. “If you’re just trying to put the puzzle together de novo, it’s hard,” she said. “But if you have a bunch of blocks you can bring into the puzzle, I think it makes it easier to put it together.”
The “Leading Difficult Conversations for Better Outcomes” course gave the physician insight into providing feedback in a way that can be heard. Dambro said when a physician was floundering within the hospital culture, she used the coursework to help align her colleague with the organization.
Dr. Jim Marshall, a pediatric critical care medicine specialist, came into the leadership program with 15 years of experience at Cook Children’s. He said the program’s mood was set from the beginning — an opportunity to learn together in a community-oriented group.
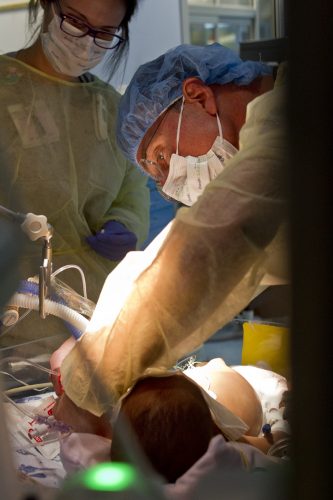
Dr. Jim Marshall, a pediatric critical care medicine specialist, works intently on an infant at Cook Children’s. He said the tone of the Advancing Healthcare Leadership program was set from the start for his group to learn together. Photo by Mark Graham
“I guess they had me at hello,” he said. “I walked into a facility that was so much better than what I was in as a college student or medical student in the ’70s and ’80s.”
The most surprising course for Marshall was the 90-minute session “Financial Acumen for Physician Leaders,” with Stephen Kimmel, chief financial officer at Cook Children’s. “I would never have expected to see a fellow come into a [room with a] random bunch of doctors and a couple of lawyers and other people in the group and just lay that all out.
“But in the context of that course, it was absolutely one of the high-water marks for me,” Marshall said. “I could see it. I could see how a health care system does this. Leaders have to lead through these changes and here was the example.”
Marshall said the program’s business-focused curriculum was the first time a leadership course had a considerable impact. “I took pages and pages of notes and went home and pet my dog and thought about stuff.”
Changing Perspective
A nurse grabbed a translucent yellow hospital gown before checking on a bald 4-year-old. The patient, eyes closed, was tucked in a tiny bed, intertwined with a network of tubes and cords.
On the other side of a tic-tac-toe-patterned curtain was a boy a couple of years older. His family talked quietly nearby. Another patient was lulled to sleep by her own heart rate monitor. Next to her bed, a nurse’s mobile computer station had a pink plastic hippo for a base. A gift bag illustrated with pastel giraffes sat unexplored on a table.
Though the atmosphere in the pediatric intensive care unit at Cook Children’s is somber, a music therapist gathered a brightly colored ukulele and hand-held percussion instruments. A drive-thru, bank-like system connected to the pharmacy shot out cylinders containing medication. A few feet away, a doctor charted from a row of computers, his speech-to-text barely audible over the muted hubbub of the unit.
A 2016 Press Ganey Engagement Survey assessed Cook Children’s employees’ opinions about their workplace. Around 400 physicians, or 74 percent, took the anonymous survey, which contained 46 questions designed to garner opinions on matters such as departmental leadership, health care system strategy and executive leadership.
Placed on the same project team, Marshall and Dambro had to interpret and communicate the survey responses. Although the assessment tool provided compelling data, Marshall, chief research officer for the health care system, was disappointed with his group’s assignment.
“Frankly, the biggest challenge for [me] came on the day that we received the project. It was like, well they already did the survey, here are the responses,” Marshall said. “We’re going to spend eight months sort of fiddling around with stuff that’s already been done.”
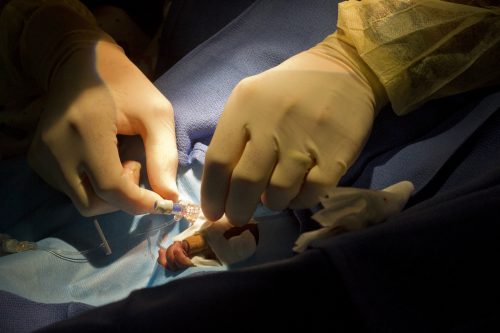
Dr. Jim Marshall performs a medical procedure on an infant at Cook Children’s Hospital. Photo by Mark Graham
After a conversation with Karla Lefebvre, director of organizational development and employee engagement at Cook Children’s, Marshall understood the scope and value of his group’s project, and he said it became a very good challenge for him.
“We needed their help,” Lefebvre said of Marshall’s project team. “Engagement survey people don’t always understand the best way to frame it — to get the physicians to absorb it, buy into it and act on it. They took this very ambiguous project and made it real and actionable. It was uncharted territory on both sides.”
Marshall’s team had to decide the best way to present the survey information and inform physicians of their standings in different categories relative to their benchmarks and other health care systems. The team also was tasked with communicating that surveyed concerns could be worked on and improved.
I think I’m a leader with more perspective now. I feel like I [better] understand how a health care system works from a leadership point of view than I did before.
Dr. Jim Marshall, pediatric critical care medicine specialist at Cook Children's Health Care System
“There was a tremendous amount of trepidation, concern for how physicians would understand the results, how they would process the data,” Marshall said. “We’re very analytical people, we’re very people-oriented, but very data-driven. Here is something that is subjective but yet objectified in numerical values. … It actually became an enormous challenge.”
From the survey results, Marshall’s project group saw gaps in alignment between hospital specialties and responses from physicians about Cook Children’s success. Group members concluded that increased transparency between hospital administrators and physicians was key in creating communication tools to use when rolling out the survey results.

Dr. Nancy Dambro laughs with Madison Gibson, an RN at Cook Children’s. Photo by Mark Graham
For Dambro, the big picture for the project group was to help medical peers understand the hospital’s overall strategy. “If people in an organization are engaged and aligned with the organization, the organization is going to be more successful.”
“[Surveyed physicians] really felt that Cook Children’s was a successful organization that was going to be here and very viable in 10 years,” Dambro said six months after retiring from her position as medical director of pediatric pulmonology. “But they didn’t have a lot of trust in the interaction between administrators and physicians, which is interesting because if you feel that something is going to be there and be successful in 10 years, you have to have some [trust].”
Since completing the leadership program, Marshall said he has seen some tangible results. “I think I’m a leader with more perspective now,” he said. “I feel like I [better] understand how a health care system works from a leadership point of view than I did before.”
Patient-Centered Care
Bouncing on his mother’s knee, a boy about 3 still wore his Paw Patrol pajamas at 10 a.m. on a weekday. His mother reminded his two siblings to stay close and keep their voices down.
“We can play right here,” the boy’s sister said to a new friend, slinging her pink blanket over her shoulder. Her mother didn’t see her daughter’s blanket dragging across a well-traveled floor in the emergency department’s waiting room at Cook Children’s.
The mother’s focus was on her toddler son, who was leaning into her lap. Her list of worries stretched beyond medical diagnoses. There was the urgent possibility of her child being admitted to the hospital. Then there were prescriptions, insurance coverage and absentee notes for her school-aged children.
What was not on that mother’s list of concerns? The technical categorization of her child as an inpatient or an outpatient.
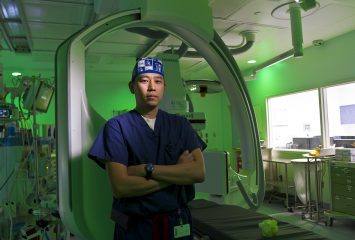
Dr. Jimmy Kuo, in a catheterization lab at Cook Children’s, delved into the handoff between physicians in the care of their patients. Photo by Mark Graham
“The movement of medicine is to separate those two [patient types] out,” said Dr. Jimmy Kuo, a pediatric interventional cardiologist at Cook Children’s. “The age of one pediatrician seeing the same patients when they are in the office and when they are admitted into the hospital is disappearing.
“There is a handoff of care,” he said. “It’s much easier to take care of the patient 24 hours a day for seven days a week, but it’s not feasible anymore.”
In the Cook Children’s leadership program, Kuo learned that the handoff is a struggle. Physicians don’t always communicate and, even more challenging, the electronic health record system categorizes a patient’s visit based on inpatient or outpatient status. The situation is like a patient having two separate files, each one in a separate filing cabinet with no easy way of combining them. “The basic idea was closing that loop,” Kuo said.
An earlier leadership team explored how to notify pediatricians that their patients were admitted to the hospital. Kuo’s project group focused on getting information about the hospitalization to the patient’s pediatrician in a timely manner after the patient’s discharge.
“Having completely separate systems is definitely a problem,” Kuo said. “Even within one subspecialty where we’re supposed to be tightknit, that could really be a problem.” His leadership group helped customize a new single-record electronic health information system.
Curriculum courses about informal hierarchy influenced Kuo’s work on his group’s communication project, and he said they continue to have applications for him beyond that assignment. “You kind of get a sense of whose opinion carries weight, whose opinion is influential, and it isn’t necessarily those who have titles.”
Focus on Quality
An elevator rang and a woman pushed a three-wheeled stroller onto the first floor at Cook Children’s. Before leaving the hospital, she decided to check out the Enchanted Castle Gift Shop. Adorned with Curious George toys, Hug a Sloth Kits and asteroid putty, the shop’s only indication of its location is the display of “get well soon” balloons.
Wearing a blue North Face fleece pullover, and carrying a Coach purse, the woman with hair in a loose bun inspected a set of bibs. In the stroller, her baby batted at colorful toys attached to the handle. Below the baby, inside the stroller’s storage basket, was a booklet entitled “A Guide for Your Journey at Cook Children’s.”
“When people go home from the hospital, we want them to stay at home and not come back,” said Dr. Karen Schultz, medical director of pediatric pulmonary services at Cook Children’s. “That would be the whole idea of getting discharged from the hospital.”
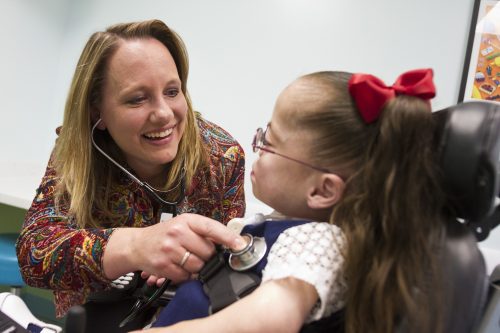
Dr. Karen Schultz, medical director of pediatric pulmonary services, listens to Faith Walthall’s heart and lungs at Cook Children’s. Photo by Mark Graham
Schultz’s leadership project team tackled the reduction of preventable readmissions. “I think we called it, ‘Get Out and Stay Out,’ ” she said. “In the literature, nobody could agree on what factors influenced whether somebody was going to come back or not.”
Cook Children’s administrators assigned this leadership project in an effort to increase quality of care and contain costs. Some medical conditions such as asthma, urinary tract infections and diabetes complications drain resources. A patient with one of these ailments is more likely to require emergency department visits and hospitalization.
Schultz’s project group met with the hospital’s discharge committee and learned that while different parts of the medical center assisted in the discharge process, those segments were not working cohesively. Instead, each hospital floor or department almost functioned as a separate entity.
“I had no idea until I did this [project],” Schultz said.
Understanding all discharge initiatives became a goal for Schultz. “I think it was awareness because there were little pockets of things going on as far as helping with the discharging: with education here, a different part of the puzzle here and a different part of the puzzle here.”
One of the project group’s recommendations was for the readmissions committee to have more physicians on it. In fact, one of the leadership program’s participants joined the committee.
I feel I am a leader now. I feel like I have new tools to be able to use.
Dr. Karen Schultz, medical director of pediatric pulmonology services at Cook Children's
Schultz said if the patient’s preferred pharmacy does not carry a prescribed medicine, a patient might not get it, especially if the significance of a specific medication is not understood. Thus, another solution from the project group: Send prescriptions to the hospital pharmacy and then provide education at that point in the discharge process.
When Schultz joined the Cook Children’s leadership program, she knew her medical career was at a transition point. She was poised to take over Dambro’s role as medical director of pediatric pulmonary services.
Schultz said she hoped the hospital’s customized leadership program would help her gain skills that she could put into immediate use. TCU business professors came through for her. When the newly installed director had to handle a conflict-resolution matter, Schultz got out her leadership course notes. The crucial conversation worked and the situation improved. At another point, her business-focused coursework on political mapping helped when a project stalled.
“I feel I am a leader now,” Schultz said. “I feel like I have new tools to be able to use.”

Your comments are welcome
1 Comment
Awe-inspiring article! I was not surprised to see Dr. Nancy Dambro or Dr. Britt Nelson.
Related reading:
Features
Physicians Find Value in Leadership Programs
Do business and leadership belong in medical school?
Features
MBA Program Advances the Business of Health Care
The degree is intended for today’s leaders in a new health care environment.
Campus News: Alma Matters
TCU Takes the Lead on Enhancing Health Care
Can leadership be taught? We think it can.