Physicians Find Value in Leadership Programs
Do business and leadership belong in medical school?
Physicians Find Value in Leadership Programs
Do business and leadership belong in medical school?
Echoes of “I wish I learned this in medical school” swirled among several Fort Worth physicians participating in two business-focused leadership programs at TCU. More than a few of them had been out of the classroom for a decade or more.
Traditional leadership seminars often were uneventful, and not nearly as in-depth and impactful as the Neeley School of Business professional leadership collaborations with Cook Children’s Health Care System and John Peter Smith Health Network.
Many of the health care professionals in the leadership cohorts said they were able to apply what they learned in a Saturday class to their work on Monday. Some even said they didn’t realize they were missing strategic management tools until they found themselves serving on committees or faced with a difficult conversation.
Some physicians didn’t even consider themselves leaders.

Dr. Britt Nelson, president of the Cook Children’s Physician Network, sits in on every session of the Advancing Healthcare Leadership program. Photo by Mark Graham
“I think contrary to what a lot of physicians feel, the minute you walk into a hospital to take care of something, people look to you as a leader,” said Dr. Britt Nelson, president of the Cook Children’s Physician Network. “Nurses want your orders. The therapists are waiting for you to say something so they can do what they need to do. The parents look at you as the leader of the team.”
Nelson attends every class of the Cook Children’s customized leadership program, Advancing Healthcare Leadership, which meets on six Saturdays and started its third cohort in August. He said he agrees with the “I wish I learned this in medical school” sentiment. “I think that’s why I keep coming,” he said. “What they teach is very valuable. I wish I had that.”
But do business and leadership belong in medical school? Dr. Jimmy Kuo, a pediatric interventional cardiologist at Cook Children’s, seemed doubtful. “When I was in medical school, everything was crammed in,” he said. “I would imagine if they tried to add [business and leadership] in, they would have to take something away.
“When the new dean of the [TCU and UNTHSC School of Medicine] came in, he talked a lot about that and I think it sounds good, but is it totally practical, especially at that time?”
Worry about learning medicine and preparing for hospital rounds fills medical students’ heads, Kuo said. For him, knowledge of the business of medicine mostly came after medical school.
But Kuo knows physicians who went to business school. “To some degree, when you go that route, you’re probably giving up some patient care and you’re probably already burnt out,” he said. “I don’t think you know whether that’s the trajectory you want to take. Until you are, I would venture to guess, [beyond] your first five years, you have no idea. Do you care about that before then?”
Double Dose of Training
By graduating medical students with insight into the business side of medicine, we hope to open minds to the myriad of possibilities to improve the human condition.
Dr. Paul Bhella, cardiologist and a professor at the forthcoming TCU and UNTHSC School of Medicine
Dr. Paul Bhella, a cardiologist at JPS, said physicians becoming frustrated with the health care system is a pathway to professional burnout. Ultimately, the goal of the new medical school is “to create physicians who will have a positive impact on the human condition,” said Bhella, who is also a professor and director of health care delivery, policy and advocacy at the TCU and UNTHSC School of Medicine, which is scheduled to open in 2019, pending accreditation.
The new medical school staff plans to incorporate leadership and business through a four-year longitudinal course composed of 10 curricular themes, such as community and public health, technology and advances in medicine, and social determinants of health.
“By graduating medical students with insight into the business side of medicine, we hope to open minds to the myriad of possibilities to improve the human condition,” Bhella said. “The practice of medicine and the opportunities to improve the human condition are both evolving — so, too, is medical education.”
In the traditional model, Nelson said, medical students don’t interact with patients and do the things they learn in medical school until their third year. “There was really no leadership,” he said of his medical school training. “What you learned about leadership was from the resident who was telling you what to do.”
Dr. Jo Anna Leuck ’00, assistant dean of curriculum at the TCU and UNTHSC School of Medicine, said the scheduling and structure of the new school’s curriculum expose medical students to broad concepts early in their education. Once students have finished their first year of clerkships (in the second year of the curriculum), that exposure expands.
But how will the new medical school conquer everything in the same amount of time as its more traditional counterparts? “The answer to this question actually goes beyond the concepts of business and leadership and speaks to the larger question: Are traditional MD school curriculums working? The answer in the literature is a resounding no,” said Leuck, who also serves as the vice chair of academics for the department of emergency medicine and the department director for the emergency medicine residency program at JPS.
Gone are the medical school days of memorizing everything, Leuck said. “Now, with the explosion in the volume of medical knowledge, as well as the ability to quickly access information, this [traditional] system is impossible and impractical.”
Instead, Leuck said her goal is to teach medical students at the new school how to formulate questions and find answers, how to apply content they read and how to be adaptable. “This approach opens up time to expand on the non-clinical but key professional skills that both patients and health care teams expect a physician to have, including leadership skills and understanding the business of medicine.”
“Physicians have always been expected to have these skills,” Leuck said. “We just now understand that they don’t occur by osmosis.”
Are traditional MD school curriculums working? The answer in the literature is a resounding no.
Dr. Jo Anna Leuck '00, assistant dean of curriculum at the TCU and UNTHSC School of Medicine
For Kuo’s first three or four years at Cook Children’s — his first job after his fellowship — he kept his nose to the grindstone. But shortly before he was selected for the Cook Children’s leadership program, he was reading books on leadership and listening to podcasts on the topic.
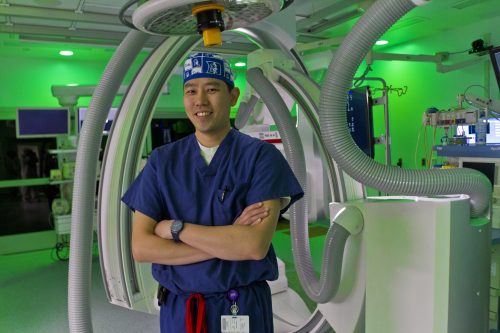
Dr. Jimmy Kuo, pediatric cardiologist, in the cardiac catheterization laboratory at Cook Children’s. Photo by Mark Graham
Kuo said he was comfortable with his medical job. Thus, he started looking up and looking around and asking questions. For the last two years, Kuo has been involved with quality initiatives and looking more critically at the heart center at Cook Children’s.
“At that point, it’s not about coming to work, doing this and going home,” said Kuo, who has been at the children’s hospital for six years. “People would say we do good work here. I would say, ‘I believe you, but how do you know we do good work here?’ ”
Putting Knowledge into Practice
For Nelson, the health care leadership programs at TCU are different: Project groups work together to solve problems and arrive at a conclusion despite disagreements. The business school’s faculty show physicians how course topics work rather than presenting a flat lecture, and the courses are customized for each cohort of participating physicians.
“You see what you just learned. You’re climbing up that mountain,” Nelson said. “I would say the other courses are complicated and this one is complex. There’s a lot of aha.”
Bhella, who completed the JPS Physician Leadership Program at TCU, said the experience gave him an appreciation of how a more global perspective can impact his day-to-day practice.
“With greater insight into the challenges and constraints of delivering health care, I am constantly on the lookout for approaches to improve how we deliver care at JPS — approaches which directly impact the care of my patients and others within the network,” said Bhella, director of cardiac imaging at JPS.
Kuo is still learning how to create change since he completed the Cook Children’s leadership program. “You have a little bit of that feeling: now what?” he said. “I think that really does fall on me in terms of what happens next.
“Hopefully these things that I’ve learned and gone through and given language to can keep on the forefront of my mind while achieving or moving us toward these ends.”

Your comments are welcome
Comments
Related reading:
Features
TCU Partnerships Shape the Future of Medicine
Leadership programs at two Fort Worth hospitals take physicians into uncharted territory.
Features
MBA Program Advances the Business of Health Care
The degree is intended for today’s leaders in a new health care environment.
Features
Stuart D. Flynn, M.D., Dean of Fort Worth’s New Medical School
TCU Magazine Editor Norma Martin spoke with Flynn about the evolution of medical school education and the opportunity to develop an innovative M.D. school in the 21st century.