Fellowship Program Trains Nurse Anesthetists to Treat Chronic Pain
The training focuses on alternative methods to help patients end their reliance on opioids.
In the small eastern Nebraska town of Albion, nurse anesthetist Steve Wooden practices as an independent pain specialist. Wooden has more than 35 years of experience in his profession, much of it spent traveling around the state’s rural areas to bring relief to patients with chronic pain.
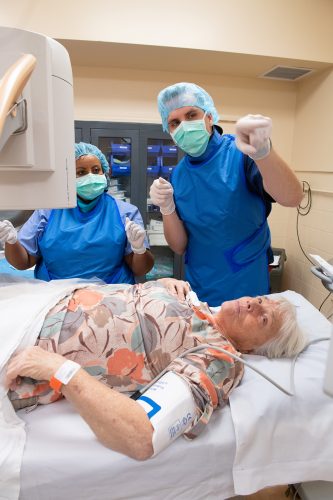
Brian H. Jacobs, a certified registered nurse anesthetist, and pain-management fellow Ruth Petros perform a medical procedure on Roberta Snyder. Photo By Joseph L. Murphy
Recently, many people who come to Wooden’s office are using prescription opioids for pain — and they are near-desperate to find another source of relief.
“Opioids have put them in a position where they have to battle with their primary care physician because they’re no longer effective,” Wooden said of his patients. “So instead of getting an additional prescription or modification, they may go out on the street and look for alternatives.”
Many Nebraskans are at risk for this pain management problem. In 2015, health care providers wrote 72.8 opioid prescriptions for every 100 Nebraskans, reports the National Institute on Drug Abuse. That year, at least 54 died of an opioid overdose, according to the state’s Department of Health and Human Services. In 2017, Nebraska received a large federal grant to respond to the crisis. Yet Nebraska is less affected by the opioid epidemic than many other states.
Since opioid prescriptions began to rise in the late 1990s, nearly 400,000 Americans have died of an opioid overdose, reports the U.S. Centers for Disease Control and Prevention. In 2016, 17,087 died from overdosing on prescription opioids — the unluckiest from among 11.5 million people misusing the drugs, reports the U.S. Department of Health and Human Services.
Many people who begin taking prescription opioids after an injury or surgical procedure wind up switching to cheaper, more easily available alternatives such as heroin to relieve pain. Those living in rural areas have limited access to pain-management doctors.

Kay K. Sanders, director of TCU’s School of Nurse Anesthesia, and Monica Jenschke, associate professor of professional practice of nurse anesthesia, help certified registered nurse anesthetist fellows learn different ways to manage chronic pain. Photo by Ross Hailey
At TCU, nurse anesthetists with expertise in pain treatment, including Wooden, are teaching colleagues to help patients with chronic pain reduce or transition away from opioids, or — better yet — to manage their pain without opioids in the first place.
The Advanced Pain Management Fellowship at the School of Nurse Anesthesia in the Harris College of Nursing & Health Sciences is one of two accredited chronic pain management fellowships in the U.S. for certified registered nurse anesthetists. The fellowship program requires hands-on clinical experiences during training.
Launched in 2016, the one-year fellowship, which leads to a certificate in pain management, empowers anesthetists to leave the operating room and tackle chronic pain using an array of tools finer than the blunt instrument of opioids.
“We’re the only [program] that’s out there really trying to deal with the opioid crisis by teaching a multimodal approach to pain,” said Kay K. Sanders ’09 DNP, director of the School of Nurse Anesthesia at TCU.
The current opioid crisis arose in large part “because providers were not trained in how to use other medications and other therapies,” said Jackie Rowles, adjunct faculty member in nurse anesthesia.
The TCU fellowship teaches a holistic approach to chronic pain, said Rowles, who also teaches nurses and medical students in Indianapolis. That includes ways to target pain at its source “and direct treatment at that pain generator — not at the symptom, which is pain.”
Monica Jenschke, associate professor of professional practice of nurse anesthesia, put it succinctly: “There are more ways to manage pain than just a pill.”
Earning Certification
TCU’s program combines online didactics by national leaders of nurse anesthesia with hands-on experience alongside anesthetists and pain physicians around the country.
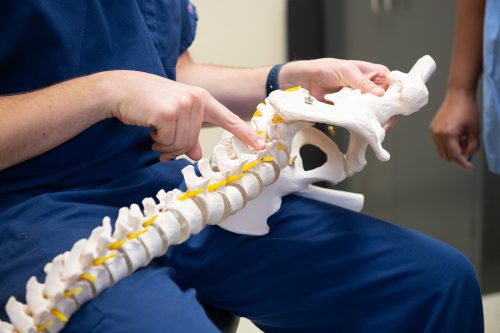
Brian H. Jacobs, a certified registered nurse anesthetist and pain-management fellow, uses a skeletal model to provide more information during a patient’s appointment. Photo By Joseph L. Murphy
Fellows review pain anatomy and physiology, learning to distinguish pain that results from injury from the kind that arises from damaged or overactive nerves. They gain advanced examination skills and study the complex psychological, cultural and spiritual aspects of pain.
The fellows also learn to recognize addicted patients; inject into painful areas; prescribe non-opioid medications, as well as opioids when appropriate; and recognize when patients might benefit from physical therapy or alternative treatments like massage. In addition to undertaking simulations, they are supervised during and evaluated on their work with real patients — 240 hours’ worth. Fellows are chosen from a pool of applicants with at least two years of experience. Most have practiced five years or more.
“We weren’t trying to take people without any background and all of a sudden magically make them chronic-pain practitioners,” Wooden said. “We wanted to find people that we felt already had an opportunity to use this education in a productive way.”
Thus the typical TCU fellow has been invited to provide pain-management services by a health care facility or a physician group but wishes to bring additional skills to the job, said Wooden, who in addition to teaching TCU students is past president of the National Board of Certification and Recertification for Nurse Anesthetists. His doctoral research laid the groundwork for the field’s new certification in chronic-pain management in 2015.
Fellows begin their experience with an on-campus orientation that includes practicing on cadavers with fluoroscopy, a continuous X-ray used during procedures such as spinal injection. Then they return to their hometowns, where they take online classes and find mentors with whom to practice their new skills. During clinical rotations, fellows track and report the cases they see and procedures they perform, such as injections of steroids to relieve painful inflammation in the sacroiliac joint, hip or spine.
TCU fellows learn three important things about opioids, said New Hampshire-based Melynda “Mindy” Wallace, adjunct faculty member in nurse anesthesia and a doctoral student in nursing practice at TCU. She has long taught a course in the Jack Neary Advanced Pain Management Workshop, which is a prerequisite for the TCU fellowship.
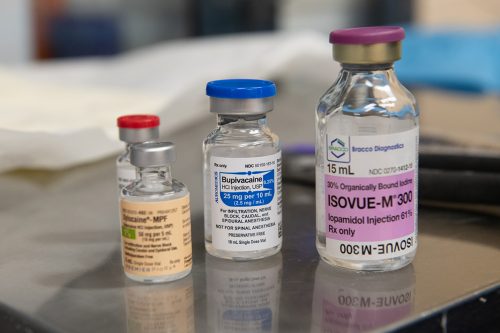
The TCU fellowship teaches a holistic approach to chronic pain, rather than relying on opiates. Photo By Joseph L. Murphy
The first is to recognize opioid addiction when they see it. Wallace asks fellows to choose an addiction screening tool and detail how they will use it, document the results and discuss it with patients. She also teaches them to interpret urine toxicology screens to help them monitor patients’ medication use.
The second is how to avoid using opioids, Wallace said. Instead, she said, “We need to be up on all the integrative methods, and when injections are working and what other medications can we use.”
Those include nonsteroidal anti-inflammatory drugs and herbal remedies, as well as more sophisticated options such as gabapentin, an anti-seizure medication that can relieve pain arising from nerves — a common affliction among, for example, people with diabetes.
Finally, fellows learn to use opioids safely and how to discuss the risks with patients.
“We need to not scare [80-year-olds who need] a couple of Percocets to stay independently living so they can do their shopping or cook for themselves and keep their house reasonably clean,” Wallace said. “We need to know how to discuss the risks with them without scaring them to death.”
After completing the program, fellows become eligible for certification in nonsurgical chronic pain management, a distinction held by about 41 registered nurse anesthetists nationally so far. TCU’s fellowship has graduated 24 students, with nine more in training.
Changing Practice
Fellowship graduates say the pain-management program has changed how they practice.
Steven W. Beckstrom, who completed the program in 2017, works in a farming area near Spokane, Washington. Many of his patients suffer from occupational injuries and lower back pain.
At first, Beckstrom attended the Jack Neary Advanced Pain Management Workshop in Chicago. There, he recalled, “[I] realized I didn’t know anything.” TCU’s fellowship “just exploded my enthusiasm to learn. … Half of [the things I learned there] I’d never even heard of when I went into the program.”
Trigger-point injections, for example, in which numbing medication and sometimes steroids are injected into tender parts of muscle, have become a staple of his practice. And learning how a variety of medications work on pain and how they affect the brain was especially helpful, he said.
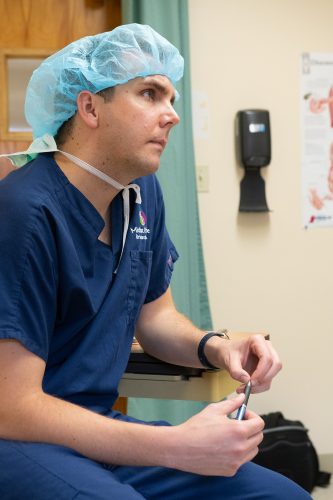
Brian H. Jacobs, who also completed the program in 2017, treats chronic pain at five clinics in rural central Iowa. Photo By Joseph L. Murphy
“Around 2007, 2008, we wouldn’t let patients leave the OR [operating room] without a bag of narcotics, and they said they didn’t have pain. And we’ve gone now to where there’s people who need it who can’t get it. We’re finding that balance,” Beckstrom said. “The program gave me the basis to study about that, to see how complicated pain really is in the human organism.
“It was so worth it,” he added. “I feel like my patients benefit every day.”
Brian H. Jacobs, who also completed the program in 2017, treats chronic pain at five clinics in rural central Iowa. His patients typically suffer from back, neck and joint pain from arthritis; neuropathic pain from diabetic neuropathy or shingles; headache; and chronic pelvic or abdominal pain. At least half are using opioids when he first sees them, but others visit him in time to avoid opioid use.
“If we can get to the patient sooner by way of referral or self-referral, then we have an opportunity to prevent an encounter with an opioid pain medication to begin with,” Jacobs said.
The fellowship program emphasizes the psychological component of pain, something Jacobs often makes use of in his practice. A lot of his patients “have a strong emotional tie” to opioids and feel that they “need those medications in the management of their pain,” he said. In such cases, Jacobs said, patients are asked to see a counselor, social worker or psychologist. After several counseling sessions, patients may start to realize that the medication was “more of a crutch” than a necessary tool to relieve pain, he said.

Monica Jenschke said the program teaches fellows to maximize inner strength. Photo by Ross Hailey
That’s why the program teaches fellows “to maximize a person’s own inner strength with meditation, yoga, stretching, physical therapy — giving them control of their own lives back,” Jenschke said.
In her practice, Rowles focuses less on patients’ pain rating and more on their ability to function. “For some of them, it’s just as simple as being able to cook dinner, being able to get on the floor with their grandkids, being able to travel to someone’s wedding,” she said. “I try to work with them to achieve that goal.”
Beckstrom said he makes a point of reassuring patients he will never stop trying to relieve their pain. “I’ve probably had 50 people cry,” he said. “They just can’t believe someone listens to them.”
Wallace said she teaches fellows when to insist that a patient seek counseling, as well as how to handle patients experiencing suicidal ideation. One of their assignments is to track down all the psychologists, psychiatrists and addiction counselors in their area who take Medicaid. Most fellows expect this task to be easy, she said. But they soon learn otherwise. Imagine attempting that search while struggling with depression or craving heroin, she tells them.
A holistic, patient-centered approach works well with nursing training, Wooden added. “The allopathic medicine model is more of a ‘name it to blame it’ pain approach — find the problem and treat it,” he said. “The traditional nursing approach is to care for the whole patient, and so understanding that patients are much more than their pain.”
And, Wooden said, “pain is so much more than a physical phenomenon.”
Finding the Right Fit
The fellowship program’s roots lie in rocky soil. For decades, TCU faculty members say, certified registered nurse anesthetists interested in chronic pain were left to their own devices, scavenging an education from colleagues and reading on their own time. Jack Neary courses have been around since 2002 but provide only an introduction to the field.
In 2011, the American Association of Nurse Anesthetists launched an online certificate program at Hamline University in St. Paul, Minnesota. By 2014, the program became a fellowship, having earned accreditation from the Council on Accreditation of Nurse Anesthesia Educational Programs.
Hamline was “trying to fly under the radar, if you will,” said adjunct faculty member Bruce Schoneboom, chief learning officer at the national nurse anesthetists’ group. He was instrumental in launching the association’s partnership with TCU.
“We knew that there would be pushback from our physician colleagues,” said Schoneboom, who also is an associate dean at the Johns Hopkins School of Nursing. “They continue the same argument: ‘You’re practicing medicine; you’re not practicing nursing. You’re not qualified.’ ”
In 2015, the association decided to relocate the fellowship, in part because Hamline had no other health care programs or an affiliated medical center. TCU, with its respected nurse anesthesia program and experience with online teaching, looked like a better fit.
Site visits went well — Wooden called TCU “a godsend” — and by February 2016, the university had signed on to a partnership with the American Association of Nurse Anesthetists. The first class of fellows matriculated that fall.

Kay K. Sanders, director of the School of Nurse Anesthesia at TCU, said the pain management fellowship teaches a multimodal approach to pain. Photo by Ross Hailey
“The resources and the individuals, the staff down at TCU have been phenomenal,” Wooden said, adding that Sanders “deserves a great deal of credit for getting this started. … We’re greatly appreciative as a profession that TCU took on this program. And we have not been disappointed in what they have done for us.”
Still, some program graduates must fight to use their skills. The issue is, in part, geographic. Some states tightly restrict registered nurse anesthetists’ scope of practice. For example, Iowa allows nurse anesthetists more latitude and independence than Missouri, a difference Schoneboom attributes to physician lobbying in the latter.
Payers and insurers also constitute “a huge artificial barrier to practice,” Schoneboom said. For example, he said, a Medicare administrative contractor may recognize and reimburse only physicians for performing procedures that registered nurse anesthetists also are qualified and permitted to do.
Jason W. Caldwell, who completed the fellowship in 2017, has run into more informal but, so far, immovable roadblocks. A resident of Floyds Knob, Indiana, Caldwell practices in Indiana and Kentucky. He holds a doctorate in nurse anesthesia practice and cited experience in regional hospitals, trauma centers and pediatric facilities, including five unsupervised years performing surgical anesthesia at a small county hospital. There, he said, nurse anesthetists “thrived,” enjoying the confidence and trust of their surgeon colleagues.
When Caldwell heard about the Jack Neary course, he contacted Rowles, who is past president of the national association and current president of the International Federation of Nurse Anesthetists. She also was one of two registered nurse anesthetists on the National Pain Strategy Team, convened at the request of the U.S. Department of Health and Human Services.
Rowles assured Caldwell that nurse anesthetists could practice chronic-pain management — something Caldwell had never heard of a colleague doing in Kentucky.
After verifying that Kentucky and Indiana both permit qualified nurse anesthetists to offer those services, though not to go into business for themselves, Caldwell attended a Jack Neary workshop. He then entered TCU’s pain-management fellowship as a member of its first class.
Although his pre-TCU practice continues apace, Caldwell hasn’t yet found employment as a pain-management provider in his area, despite presenting his credentials to many small hospitals and private-practice physicians.
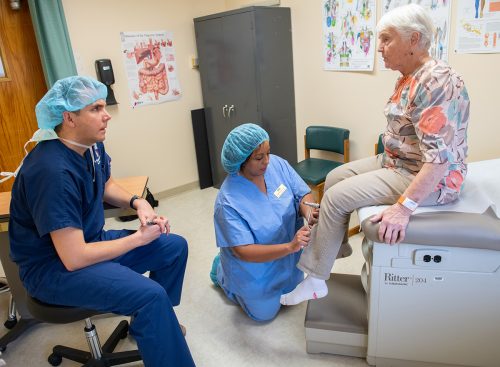
Roberta Snyder (right) discusses the amount of pain that she feels as Brian H. Jacobs and Ruth Petros perform an exam at the Guthrie County Hospital in Guthrie Center, Iowa. Photo by Joseph L. Murphy
“In Kentucky, pain practice is heavily physician-dominated,” Caldwell said. In many of the facilities where he provides sedation, he added, doctors give him “the pat on the back. … You know, you kind of get the ‘Hey, man, that’s nice! But don’t come near our territory.’ ”
But skeptical pain-specialist physicians ought to look at the TCU curriculum, Caldwell said: “Compare the didactic portion to theirs and just see what we accomplished in a year’s time. It’s amazing. I think my education, my fellowship, I think it was on par with a medical fellowship. … To me, personally, it was worth it.”
Essential Service
Geography — specifically, the urban-versus-rural divide — is among the reasons some experts say registered nurse anesthetists should be permitted to practice according to their training.
The opioid epidemic is raging in rural areas, where nurse anesthetists are often the sole providers of anesthesia services. A 2011 study by the Rand Corp. found that rural health care facilities are likelier to employ anesthetists than anesthesiologists (who are paid, on average, twice as much).
Joanne Spetz, who studies the economics of the health care workforce, is the associate director for research at the Healthforce Center at the University of California, San Francisco. She said the timing is good for a fellowship like TCU’s program.
“Nurse anesthetists are absolutely essential in rural communities, and we know that the overdose rates and so on are higher,” Spetz said. “Many of those communities have a job base that is more heavily in the manual labor field,” with high occupational injury rates.
“Recovering from that involves a lot of chronic-pain management skills,” she added. “You’re going to be very reliant on nurse anesthetists.”
Adam Millsap, an expert in state policy at Florida State University, wrote in an email that having more health care professionals makes it easier for patients to find caregivers and keep costs down. He added that insurance is one of a number of ways to alleviate training or safety concerns apart from outright scope-of-practice bans.

Ruth Petros holds Roberta Snyder’s hands during an exam at the Guthrie County Hospital in Iowa. TCU’s Advanced Pain Management Fellowship helps nurse specialists like Petros use a patient-centered approach to pain management. Photo By Joseph L. Murphy
“Increasing the supply of people who can help opioid users deal with chronic pain should improve the situation,” Millsap wrote. “Better monitoring of opioid use may prevent some addictions, and it’s easier to monitor when there are more people doing the monitoring.”
Nurse anesthetists who complete specialized training in pain management should be able to provide such treatment, wrote Edward Timmons in an email. He is the director of the Knee Center for the Study of Occupational Regulation at Saint Francis University in Pennsylvania.
State occupational laws restricting practice are “particularly problematic in rural areas where patients may have to drive an hour to see a doctor,” Timmons wrote. “Offering more patients the opportunity to seek out additional treatment options for pain management seems like a step in the right direction.”
Tipping Point
Wooden said he understands naysayers’ desire to ensure that people providing pain management can do it safely and well.

TCU’s pain management fellowship helped Ruth Petros learn about alternatives to opioid use to help patients like Roberta Snyder manage chronic pain. Photo By Joseph L. Murphy
Pain management fellowship programs such as TCU’s may lead to “a tipping point, where it becomes recognized that this formal education program is the pathway to providing chronic-pain care in this country,” Wooden said. “We want to be able to expand to the point that other universities see the value and offer similar programs.”
In the meantime, Schoneboom said, the American Association of Nurse Anesthetists has good data to support the safety and efficacy of nurse anesthetists’ pain practices, though many of those data remain unpublished, a situation he’s determined to fix. The association is building a national outcomes database, he said. It also works with payers to introduce provider-neutral language into chronic-pain management documents.
No single discipline owns pain management, Rowles said — not medicine, not physical therapy, not psychology. “A pure multimodal approach has been shown to be best for our patients,” she said. “We all have to work together. It’s not easy. But I think as we can demonstrate our knowledge, skills, education and competency, then things should continue to improve for us.”
Jacobs, too, believes pain is everyone’s business. “Everyone needs a better understanding of patients with pain,” he said. “We need to better recognize the effect that pain is having on the patient and intervene sooner, so that the patient can get back to living a meaningful, purposeful life.”

Your comments are welcome
15 Comments
I’m interested
Im very interested and I do have some questions.
Wow a whole 240 hours?! So three weeks of medical school worth of actual supervised training. This is such a sham and dangerous for patients.
It’s quite laughable to compare this certificate program to a legitimate pain fellowship. Especially since pain fellowships are completed AFTER a 3-4 year medical residency.
“In addition to undertaking simulations, they are supervised during and evaluated on their work with real patients — 240 hours’ worth.“
“Compare the didactic portion to theirs and just see what we accomplished in a year’s time. It’s amazing. I think my education, my fellowship, I think it was on par with a medical fellowship.”
If you really think this is true, you need to go do a medical residency and fellowship. I’m usually sympathetic to CRNAs, but this comment is a joke. I did more than 500 hrs of work in a chronic pain clinic during residency alone (I didn’t do a fellowship, and don’t perform chronic pain procedures in my practice). Fellows in pain medicine are in general going to have an additional 2000+ hrs working directly on patients, in addition to didactic training.
Lost me at online…and equivalent to physician. Laughable
Because this fellowship is obviously equivalent to 4 years of medical school, at least 4 years of residency, and a year of fellowship. If you want to do physician tasks, then go do the PHYSICIAN route.
Also, it sounds like a good chunk of this training is online. What would be your thoughts if your surgeon did most of his/her training online. That concern is also relevant to this program. Doing spinal steroid injections can alleviate back pain if done correctly, but it can also cause paralysis and even a stroke if done incorrectly. There is so much risk and patient endangerment involved if this program expands and gets more recognition.
How is it even legal?
What a money-grabbing scam. 240 hours training and you know enough to prac Nonsense!! MD’s spend 10,000 hours over 5 years following their MD degrees to do this. And MD’s trained in pain aren’t pushing opiates either.
What a terrible idea. Far beyond their scope of practice and extremely dangerous for patients.
CRNAs belong in the OR; they need to practice within their scope. The only reason they want to do procedures is for the money. Let’s be honest. The answer to the opioid crisis is NOT to have a bunch of burnt out CRNAs leave the OR so they can do procedures they have no business doing. I am double board certified in PM&R and Pain Medicine. The bulk of my 3 year PM&R training focused on musculoskeletal and neuromuscular medicine (including becoming proficient in electromyography and musculoskeletal ultrasound). That made me an expert in diagnosing the very wide variety of pain conditions. My pain fellowship was extremely diverse and included hundreds of proctored fluoroscopic procedures of the most complex variety. The ignorance of the author of this article is glaring. Although pain procedures are one tool to treating pain, they are far from the solution and will NOT be the answer to ending the opioid crisis. The crisis is far more complex than that. Having a bunch of poorly trained CRNAs doing spinal procedures that can have catastrophic consequences if done incorrectly is NOT the answer. If you are a nurse and want to do pain management, then don’t become a CRNA. You should become a general nurse practitioner and then go work in a pain clinic under the supervision of a board certified pain doctor; you have no business EVER doing fluoroscopic spinal procedures. Otherwise, what’s next? An online course for CRNAs to do spine surgery??? I guess since CRNAs do anesthesia for spine surgeons on occasion that should make them qualified to do surgery with a “comprehensive” online course too, right??? This “training program” is a joke and is reckless. Stay in the OR where you belong!
I have 27 years of healthcare experience, 5 years cardiac-tele, 7 years ICU experience in Minneapolis, and 15 years experience as a CRNA.
“CRNAs BELONG IN THE OR; THEY NEED TO STAY WITHIN THEIR SCOPE OF PRACTICE.”
I work for the United States Federal Government Indian Health services. I work 80 hours a week and I am on call 24 hours a day then trade with another CRNA who does the same. Yes, we cover the OR, but we also cover the floor, we also insert epidurals and spinals, do anesthesia for emergency c-sections, emergency intubations, trauma codes in ER, Code Blue in ER, vent management in ER,
assist flight teams with emergency care, assist in loading patient’s on the helicopter, the other CRNA does epidural steroid injections and I am sure I am missing a lot of other functions we participate in.
So when I see “CRNAs BELONG IN THE OR; THEY NEED TO STAY WITHIN THEIR SCOPE OF PRACTICE” I find this very belittling and take great offense to this. I serve my country as a SOLO CRNA. I also serve the FIRST NATIONS PEOPLE of this country who were promised healthcare. Without CRNAs THE FIRST NATIONS PEOPLE would be getting none of these services!!!
When I see “CRNAs BELONG IN THE OR; THEY NEED TO STAY WITHIN THEIR SCOPE OF PRACTICE” reminds me of the saying “WOMEN NEED TO STAY IN THE KITCHEN”.
I am interested in a pain fellowship but do not have a mentor. I know where I work the people could greatly benefit from someone trained in pain management. Is there anyway of taking a pain fellowship without having a mentor?
I mean to say a Mentor at your location.
Wow, a whole 6 weeks of supervised training in pain diagnosis and treatment. This is not anywhere close to the training that MD’s and DO’s undertake! 4 years of medical school, 4 years of residency and 1 year of fellowship. This is a nice little scam to to allow undertrained and inexperienced mid-level providers to jump the line and practice subspecialty medicine. When the extent and breadth of the training program and the board certification requirements are equal to those for physicians, then it might be worthwhile, but this is just cheap labor for a “training” program and foists marginal providers on an unsuspecting public. Providing less skilled providers to work in the offices of orthopedic surgeons performing procedures whose potential complications they cannot fully evaluate and treat is just shameful.
Related reading:
Campus News: Alma Matters, Research + Discovery
Hands-On Learning Helps Medical Students Put Patients First
TCU and UNTHSC School of Medicine’s Dr. Stephen Scott discusses the school’s integrated approach to education.
Campus News: Alma Matters, Research + Discovery
Mauricio Papini: Looking for the Link
The psychology professor says addiction, pain and frustration have something in common.
Features
TCU Partnerships Shape the Future of Medicine
Leadership programs at two Fort Worth hospitals take physicians into uncharted territory.