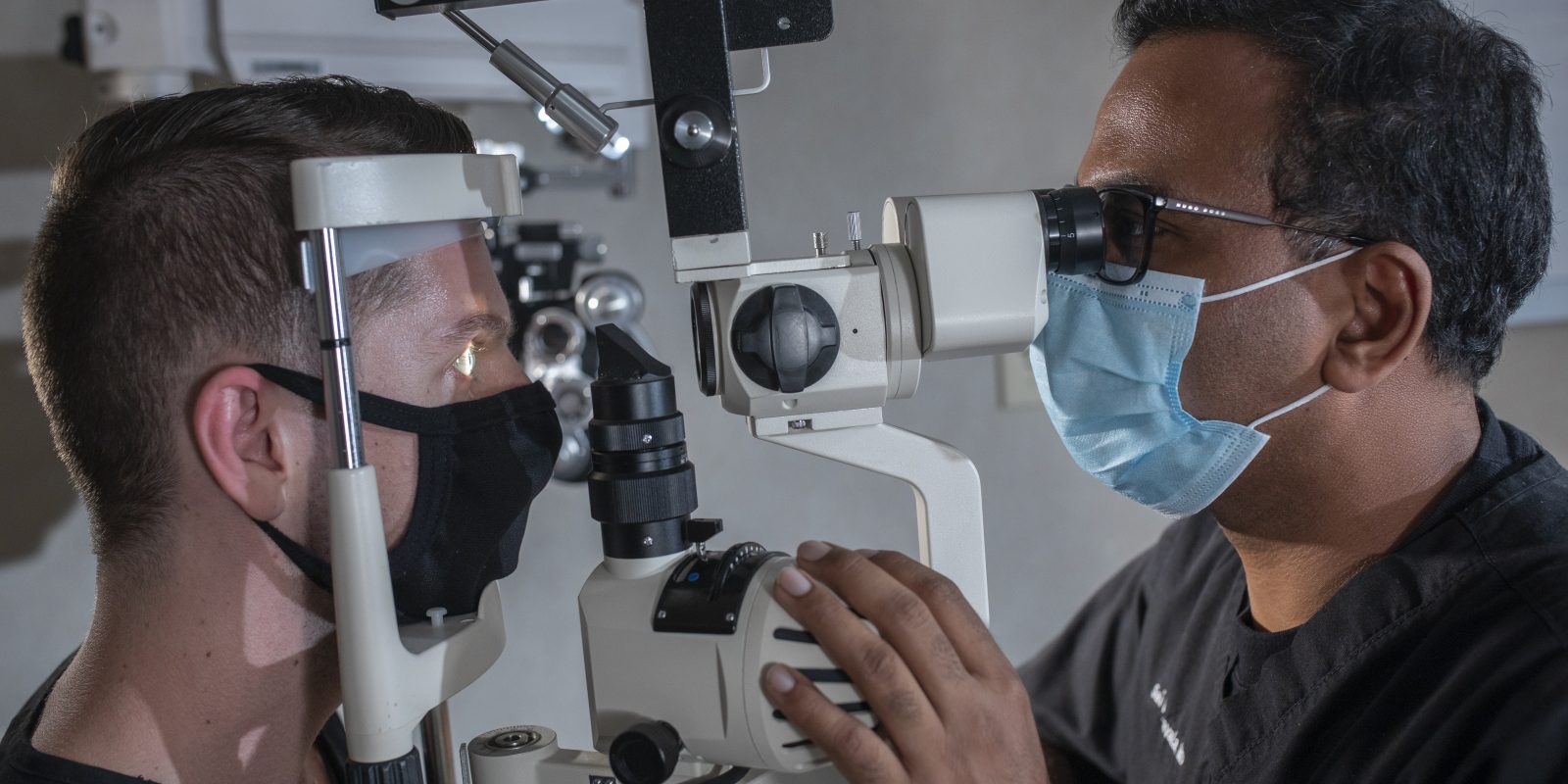
Dr. Sai Chavala is a retina specialist and professor of surgery at the TCU and UNTHSC School of Medicine. Photo by Rodger Mallison
Reprogramming Cells Could Restore Vision
Sai Chavala’s new research puts hope in sight for people with macular degeneration.
Driving to the neighborhood grocery store or filling in a crossword puzzle are routine activities many people take for granted. But imagine the limited possibilities — and shock — for people who lose their vision.
About three years ago that became a reality for Bobbie Krusz, now 97, of Dallas when she was diagnosed with macular degeneration, an incurable disease that guaranteed her vision would decline.
“Learning that I was losing my vision was the most devastating news,” Krusz said. “Your vision becomes blurry, and then it would seem to be OK for a little while and then blurry again. You love the freedom [vision] gives you. We don’t realize how liberating it is until we can’t do it anymore.”

Dr. Sai Chavala and his team identified a new method to alter cell identity and reprogram skin cells into retinal cells. Photo by Rodger Mallison
In July, Krusz was accompanied by her daughter, Pamela Krusz, for a midmorning appointment with Dr. Sai Chavala, an ophthalmologist and professor of surgery at the TCU and UNTHSC School of Medicine. They were visiting KE Eye Centers of Texas in Dallas for Bobbie’s quarterly injection in her left eye.
“The whole process is a little bit stressful because none of us want to get a needle in our eye,” Pamela Krusz said.
Macular degeneration, caused by the loss of photoreceptor cells, is the most common form of age-related vision loss. Those photoreceptor cells are responsible for converting light into signals that are sent to the brain. Photoreceptors give people color vision and night vision.
People can experience dry macular degeneration or wet (neovascular) macular degeneration, which happens when blood vessels grow under the retina and leak. The latter is rare and typically happens suddenly.
The more common form is dry macular degeneration, in which vision loss happens over several years. The disorder is more common in people over 50 and in Caucasians, reports the Mayo Clinic. Research has shown that family history and genetics, obesity, smoking and cardiovascular disease are factors in developing dry macular degeneration.
“For that form of macular degeneration there is no therapy. There is no treatment,” Chavala said. “It’s frustrating for me because patients come to the clinic looking for hope, and we’ve got nothing to offer. You’ve got people who have worked 30-40 years and are ready to enjoy retirement, and then all of a sudden you get dry macular degeneration and you can’t see. I was inspired to become a physician-scientist to try to solve this problem.”
That quest led Chavala and a team of researchers from the University of North Texas Health Science Center and North Texas Eye Research Institute to what they believe is a solution to this medical conundrum: changing skin cells into retina cells.
Skin cells possess most — if not all — of the genetic material present in essentially any cell in the body.
Skin cells are of great interest in medicine because they are easily accessible and have the ability to regenerate. A core question in Chavala’s research is the determination of cell identity: Why is a skin cell a skin cell, and can a cell’s identity be changed?
Skin cells possess most — if not all — of the genetic material present in essentially any cell in the body. The active genes that give skin cells their identity are present in the unwound, open areas of the chromosomes. In the closed, tightly wrapped areas, there are inactive genes that normally make a liver, a heart, an embryonic cell or an eye cell.
Chavala and his team identified a new method to alter cell identity and reprogram skin cells into retinal cells. The direct reprogramming involves bathing the skin cells in a cocktail made up of five small molecule compounds. Together the compounds act as a construction crew, closing and opening new areas of the chromosomes and activating new molecular pathways. The result is the creation of rod photoreceptors that mimic in appearance and function the innate rods that normally develop on the outermost layer of the retina.
“We hope these chemically engineered skin cells can be transplanted into the retina for a myriad of diseases, such as macular degeneration, where photoreceptor deficiency leads to vision loss,” Chavala said.

Dr. Sai Chavala discusses a a retinal scan with Tori Paugh, a certified ophthalmologist assistant. Chavala’s team is trying to change skin cells into retina cells. Photo by Rodger Mallison
For proof, Chavala transplanted engineered skin cells into the outer retinas of blind mice. One month later, the mice were able to detect light, and their natural fear of lighted spaces was restored. The researchers also demonstrated that human skin cells, from both healthy and vision-impaired donors, could be used to generate photoreceptor-like cells, and transplantation of these cells into blind mice also led to functional improvement.
Results of the study, for which Chavala served as the lead investigator, were published in Nature in April.
“Our field of medicine [ophthalmology] is a bit underrepresented in scientific research, and there are few studies related to vision that are published in the journal Nature every year,” Chavala said. “To have one of these come from our research lab is a true honor.”
The idea for this type of eye research has been explored by popular TV. It was a plot point on CBS’ hit sitcom The Big Bang Theory during its 10th season in an episode called “Brain Bowl Incubation.”
When the episode begins, two of the main characters, Amy and Sheldon, are in Amy’s research lab, where she takes skin cell samples from Sheldon’s arm and attempts to convert them into functioning brain cells. Later in the episode, Sheldon is thrilled to find out that Amy’s experiment worked.
“It’s interesting that what those fictional characters were conversing about was the concept of sidestepping stem cells,” Chavala said, “which is what our team demonstrated in the Nature paper.”
Bypassing stem cell conversion offers an advantage because differentiating those cells into the desired end products can take six or more months. The researchers’ skin cells were transformed into functional photoreceptors and ready for transplantation after 10 days.
“I feel very encouraged, and with Dr. Chavala, I feel like there is a light at the end of the tunnel and a lot of hope.”
Pamela Krusz
The breakthrough benefits patients and physicians in training at the TCU and UNTHSC School of Medicine.
“Dr. Chavala’s work represents a significant advancement in the worldwide challenge to address retinal disease and blindness,” said Dr. Stuart D. Flynn, the medical school’s founding dean. “This work is a wonderful model for our students as they learn and experience the robust interface between the science and art of medicine, always with the focus on the patient.”
For patients regularly visiting Chavala’s clinic, like Bobbie Krusz, a cure for dry macular degeneration would mean a restoration of freedom.
“Hearing about his research made our day,” said Pamela Krusz. “I feel very encouraged, and with Dr. Chavala, I feel like there is a light at the end of the tunnel and a lot of hope.”
The next step for Chavala and his team is to work toward Food and Drug Administration approval, which is expected to be a two- to three-year process if adequate funding can be obtained, before the eye cell treatment can be studied in a clinical trial. The team also has made strides in developing the skin cell technology to benefit patients with glaucoma.
“Vision loss is all about quality of life, and that’s extremely important,” Chavala said. “I want my patients and the public to know that there is hope in sight.”

Your comments are welcome
11 Comments
todo bien
I have advanced wet macula degeneration for 4 years I am 71 years old can u help me I get shot in my eye every 8 or 9 weeks
Will this be effective in Myopic macular degeneration?
Wry interested in cell activation for dry macular. Are there human trials?
Just diagnosed dry! Any trials in UW WI Madison?
I hope you will continue to use this for wet macular degeneration in which I have had since I was 60 years old. I am now 66 and am scared it is going to get worse.
Will this be able to help glaucoma patients. Ihave lost vision and night vision ..
This is the sad paradox of American medical research & medical discovery
If this project were continued in Europe, Australia,Germany, Japan , it could be in use & on the market in perhaps a YEAR . Because American medicine is bogged down with lack of funds, & stalled out, overburdened research requirements we lose out. The process becomes politicized , obbied etc. Get this DR & team the money & country to advance this in a reasonable time ..!
I hope thisreatment. Ccomes soon to public. I too have amd
I have a 91 yo mother who is physically and mentally fit. The only thing keeping her from living a full life to 100 is loss of eye sight from MD. She gets a shot in one eye every 4 weeks. The other eye has not shown any improvement from a shot so the doctor is no longer treating that eye. Would love to know when you will start trying this on humans? God bless your research.
I pray this will work , I have DAMD and very scared of becoming blind
Related reading:
Alumni, Features
Lighthouse for the Blind CEO Saw the Possibilities
A varied career in business took Platt Allen from data systems, to entrepreneurship, to helping the visually impaired reclaim their lives.
Campus News: Alma Matters
Dr. Terence McCarthy Leads New Medical School’s Emergency Program
The doctor is the John M. Geesbreght MD, MS, FACEP Chair of Emergency Medicine — the first endowed chair position at the TCU and UNTHSC School of Medicine.
Features
Creativity Boosts Your Brain
Art helps the brain stay healthy, which leads to a thriving life.