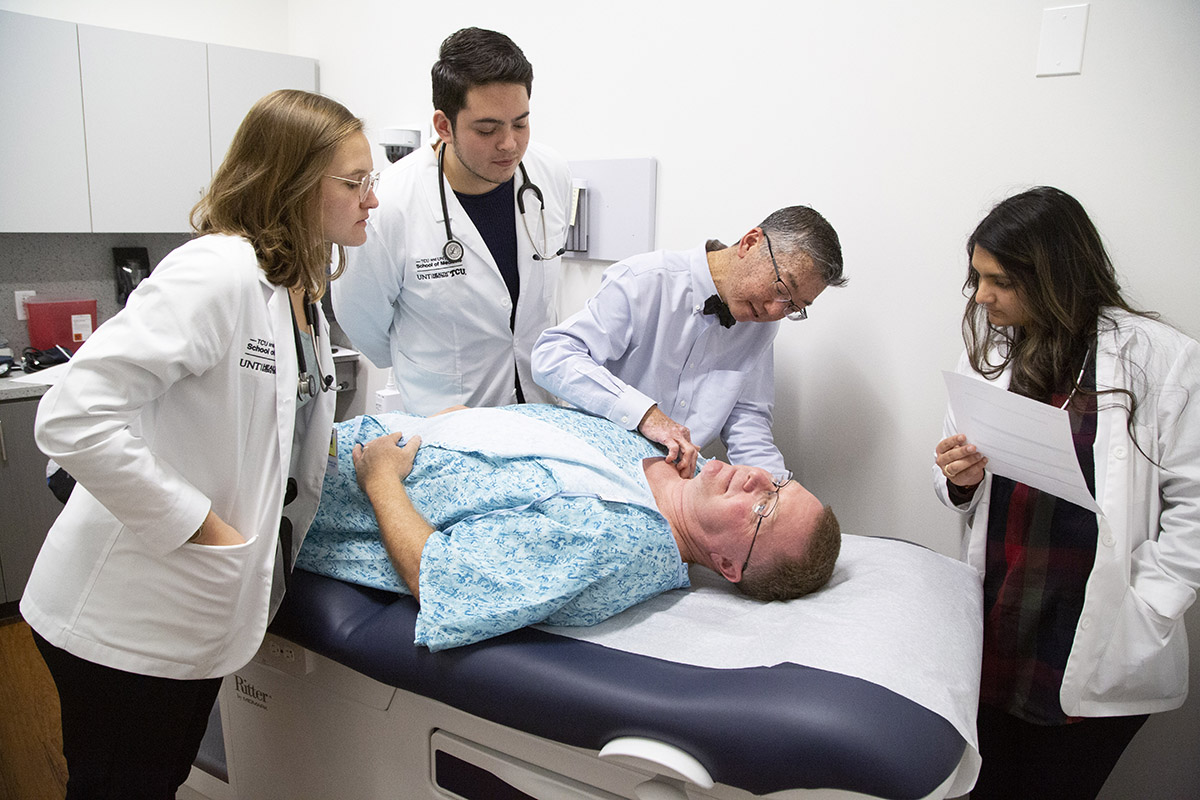
Students Shelby Wildish, Edmundo Esparza and Juhi Shah watch as instructor Dr. Song Lee teaches in the clinical skills lab with patient Chris Clark. Photo by Joyce Marshall
New Fort Worth MD School’s Students Finish First Year
The first year in the lives of six students from the TCU and UNTHSC School of Medicine’s inaugural class was marked by innovation and pivots.
Two hours after grabbing a breakfast burrito one morning in early March, Jonas Kruse removed the top of a skull.
He and his classmates were three days into neurology, considered among the most challenging disciplines that medical students in the U.S. encounter during their first year.
Despite the chilly temperature in the cadaver lab, Kruse brought intensity and focus to the task. His hands did not shake. His stomach never quavered.
 “That night I was thinking how I took a brain out of a human head at 9:30 a.m., and it was sort of business as usual,” Kruse said. “It’s surprising what you can actually get accustomed to.”
“That night I was thinking how I took a brain out of a human head at 9:30 a.m., and it was sort of business as usual,” Kruse said. “It’s surprising what you can actually get accustomed to.”
Back in summer 2019, most of the students at the new medical school — a joint venture between Texas Christian University and the University of North Texas Health Science Center — probably considered sawing into a body anything but routine.
In fact, Edmundo Esparza felt shattered upon initially encountering his cadaver, a 70-something-year-old male who had died of kidney failure.
“The body feels very stiff,” Esparza said. “I don’t know why, but I always expected it to feel more natural.”
No one could have known that the day the students removed brains would be the last time they’d see their cadavers during their first year at the School of Medicine, which opened in July 2019.
As a result of COVID-19, the class would not come together on campus again during the academic year.
But thanks to a pioneering curriculum that focuses on empathy and communication, the school was poised to address student needs and propel their medical education forward, said Dr. Stuart D. Flynn, the school’s founding dean.
The pivot to an online-only curriculum enabled the students to keep up an intense pace, one that puts them on a path to becoming doctors in May 2023.
Warm Welcome

Jonas Kruse and Quinn Losefsky happily donned their new white coats in a celebration with friends and faculty in July 2019. Photo by Mark Graham
On July 27, 2019, a morning filled with sunshine and promise, Kruse took the stage in TCU’s Brown-Lupton University Union, the slight flush on his cheeks more from excitement than nerves.
He stood before a crowd that included his wife, as well as parents and stepparents who had flown in from Southern California. The ballroom thrummed with the energy of fellow students supported by their own families and friends.
Everyone had come together to celebrate the inaugural class of the TCU and UNTHSC School of Medicine, the first new medical school in Fort Worth in a half-century.
“It’s truly humbling to think about how much has been invested in us,” said Kruse, elected by his peers and faculty to speak on behalf of the class at the white coat ceremony, a rite of passage for new health care students.
“It took an army of individuals to get us here,” he said, “and we’re all really excited to be a part of this cutting-edge school.”
As the audience cheered, Flynn beamed from the podium. Hired in 2016 to lead the effort of opening the school, Flynn also has taught surgery and molecular pathology at Yale University and served as founding dean of the University of Arizona College of Medicine-Phoenix.
Flynn nodded to Kruse as he stepped off the stage and took his place beside Quinn Losefsky ’19.
Earlier in the ceremony, Losefsky had helped honor H. Paul Dorman, chairman and CEO of DFB Pharmaceuticals. The Fort Worth businessman and philanthropist donated the first full year of tuition, which amounted to $57,500 for each of the 60 aspiring doctors in the room.
“I understand the need for exceptionally trained physicians,” Dorman said, “and I believe the TCU and UNTHSC School of Medicine team is creating the right formula to prepare students in the practice of medicine in the future.”
Within minutes, students were untying the silver ribbons on shirt boxes, the vibe more kid-on-Christmas-morning than high-achieving scholar.
Tears, hugs and high-fives followed as the first-years slipped on their white lab coats.

Quinn Losefsky and H. Paul Dorman talked before the July 2019 white coat ceremony. Losefsky helped honor Dorman, a Fort Worth businessman and philanthropist, who donated the first full year of tuition for each of the 60 medical students. Photo by Mark Graham
Losefsky, one of a dozen TCU graduates enrolled in the inaugural class, found herself anticipating what the next couple of months would hold.
She was drawn to the fact that, unlike their peers at most medical schools, students at this school would begin to see patients almost immediately.
During year one, which concluded at the end of June, Losefsky and her classmates learned about more than anatomy, physiology and disease. They convened as a class, in small groups and one-on-one with physician-mentors to wrestle with big problems from difficult diagnoses to the future of medicine.
The implications of their chosen profession would hit the students in waves as they attended class, studied and volunteered in the community. The coronavirus pandemic highlighted the risk to practitioners, particularly those on the front lines.
The COVID-19 crisis also served as a stark reminder of projected physician shortfalls nationwide. Research from the Association of American Medical Colleges indicates the U.S. could need 122,000 more doctors than it will have by 2032.
Big Dreams
For Losefsky, pulling on the lab coat was the realization of a dream that had propelled her since her teen years.
When the eighth grade science class at her school in Austin, Texas, dissected a cat, no one else in her group would touch it. The teacher saw what she’d done and declared it the best dissection he had ever seen.
“That was when I knew I was going to be a surgeon,” Losefsky said.

Charna Kinard, right, laughs with classmates. She said she wants to be a surgeon. Photo by Mark Graham
Charna Kinard, who graduated from Loyola University in Chicago, also intends to go into surgery. She began considering a career in medicine at age 11, when she lost a grandmother to mesothelioma, a type of lung cancer related to asbestos.
Both Ivette “Ive” Mota Avila, who was in Kinard’s class at Loyola, and Esparza, a University of Texas at El Paso grad, earned MBAs before heading to medical school.
In middle school, Esparza followed his older siblings’ path: cutting class, causing trouble and underperforming. He was on the verge of failing eighth grade. Because he often finished standardized tests before his classmates, a teacher gave him a copy of the first Harry Potter book.
As he tore through the series during the summer before high school, Esparza asked himself why he was acting out.
He identified with the popular novels’ main characters as they demonstrated intelligence and resilience by overcoming odds again and again. He found delight, too, in reading about the positive exchanges between young wizards and the staff at their school, Hogwarts.
“I was just being dumb, ditching with friends,” Esparza said, “but I liked school.”
Well, maybe not learning about kidneys. Few of the medical students seemed enamored with the study of nephrology, but Esparza found the experience painful.
His father’s Type 2 diabetes had gone unmanaged for years. Mundo Esparza developed diabetic neuropathy, which his son described as damage to the nerves resulting from unchecked high blood sugar. That in turn harmed his kidneys.

Edmundo Esparza joins classmates in a simulation classroom. Photo by Joyce Marshall
“Everything spun off the diabetes,” Esparza said. His father’s brain also stopped working correctly, as did his heart.
Since Esparza’s father had served in the Mexican state police, he was eligible for care at a state hospital over the El Paso border. But there he was misdiagnosed.
Moreover, the byzantine health care system in Mexico meant that the doctors dealt only with the presenting symptom.
So when the elder Esparza went to the hospital for heart palpitations, his medical team would look at nothing beyond that. When he developed an infection in the hospital, they had to discharge him for the heart problem before readmitting him for the new infection, a process that might take anywhere from hours to days.
“These things are so easily taken care of here if you have the money,” Esparza said. “There was no reason for the progression, let alone the outcome.”
The family buried Mundo Esparza on March 1, 2018.
His youngest son started medical school 494 days later.
Exemplifying Empathy
Medical student Dilan Sunil Shah spent two weeks in summer 2019 at a silent meditative retreat on the Indonesian island of Java to prepare for the classroom.

McKenna Chalman and Dilan Shah work through instruction with a model heart. Photo by Joyce Marshall
The outgoing Shah, who aims to become a psychiatrist, believes he can help people manage emotions at a time when the National Institute of Mental Health reports rising rates of suicide.
The increase disproportionately impacts health care professionals, particularly those in training. A 2019 report from the American Medical Association revealed that medical students “are three times likelier to die of suicide than their counterparts in the general population.”
Days into medical school, Shah and his classmates spent a morning with professors and other staff for an introduction to The Compassionate PracticeTM which Flynn described as communication skills training embedded into the school’s curriculum.
In September, the students received diversity training with an emphasis on microaggressions and how biases in race, gender and sexuality might affect care.
Kinard embraced recommendations on how she should introduce herself to patients. She began most patient encounters by saying, “My name is Charna Kinard, and I use the pronouns she, her and hers. What are your pronouns that you prefer me to use?”
“Sixty-four percent of patients say they have had a health care experience with a meaningful lack of compassion, one that impacts their health,” Chase Crossno told the students during the first week of school.
As the medical school’s assistant artistic director, Crossno crafts student experiences that use improvisational, role-playing and storytelling skills more typical of a theater curriculum.
As part of mandatory monthly reflections, students wrote about how they felt about patients and classes.
“We can use it as a way to talk through the anxieties we have felt when we’ve asked a patient about something really personal,” Esparza said. “It’s part of learning how to deal with the responsibility that comes with being a doctor.”
In other assigned writings, students might take the perspective of a patient as a way to increase sensitivity for those suffering.
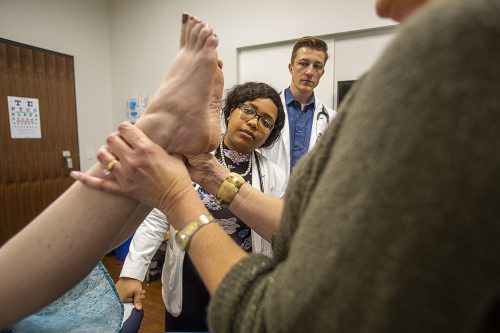
Medical students Charna Kinard and Jonas Kruse watch an examination during a clinical skills session. Photo by Mark Graham
“For so many years, I’d been told you can’t wear your feelings on your sleeve to be a doctor, that you have to have distance between the patient,” Kinard said. “But the storytelling and small groups we have at this school give us the chance to see that’s wrong.”
In a move to de-emphasize stress and competition while enhancing collaboration, the curriculum is pass-fail throughout all four years. Also absent are traditional ranking systems.
“It only serves to hurt the collective if someone else is struggling,” said Kruse, who noted that during the first semester he received daily group texts from fellow students asking questions or sharing resources.
“There are no classic gunners here, the kind of med student obsessed with being No. 1,” Losefsky said. “We don’t have a No. 1.”
The together-we-rise ethos has a practical side, too: The startup school’s national ranking will hinge to a degree on how well the group performs on the United States Medical Licensing Examination, which every MD in the U.S. must pass before being licensed to practice.

Six TCU and UNTHSC School of Medicine students allowed TCU Magazine to follow them through their first year of medical school. Photos by Mark Graham
A Rapid Transition
In response to the COVID-19 pandemic, the school went entirely online. The initial announcement of the suspension of in-person classes and on-site patient interactions came in mid-March, toward the end of spring break.
To blow off steam after an intense winter that included physics-laden pulmonology, Kruse, Shah and six other students had traveled to Disneyland and the beach. Most devoted the mornings of their California vacation to reviewing medical terms.

Ive Mota Avila gets ready to walk Blue, left, and Winter, before studying in her RV home. Photo by Joyce Marshall
Avila, who owns a small ranch in Austin with her husband, Sam, had joined him on a road trip around the state.
She and Sam had purchased a fifth wheel, a type of RV pulled by another vehicle. The couple intended the move as a way to economize on rent over the four years that compose a doctor’s undergraduate medical education. At the end of the holiday, she resumed her studies in Fort Worth alone in the camper.
Despite agonizing over whether to return to Austin, Avila knew that on the ranch, “I am someone else with other responsibilities.
“Thinking about going home and having those two different identities meet and get along is very stressful and scary for me.”
Avila decided not to risk returning to the ranch to finish her first year. Instead she stayed in Fort Worth and kept her focus on medical school.
Kinard was returning from a conference in Kentucky with her mother when she learned of the delay in returning to campus because of COVID-19. She struggled at times to process the implications of the pandemic.
Keeping up with endless news cycles while diving back into her studies — particularly rigorous neurology — seemed overwhelming, she said.
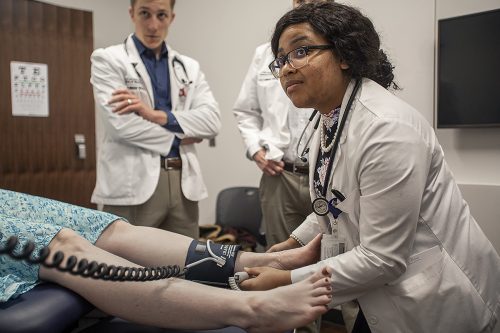
Charna Kinard practices an examination on a patient. Since the coronavirus pandemic prevented in-room visits, Kinard said online learning has its shortfalls. Photo by Mark Graham
The School of Medicine’s transition to virtual classes was made somewhat smoother by the fact that independent learning in a team setting resides in its DNA. But many, Kinard included, acknowledged the challenges of connecting online.
“When we’re working together on Zoom, people are much quicker to shut someone down or dismiss them,” Kinard said. “The goal was always to raise each other up, but I do feel the distance has taken away some of the common considerations we would give each other in person.”
Like other classmates, Kinard longed for a return of in-person dynamics. A gamer who has competed in multiple tournaments, both solo and as a member of a team, Kinard played cards with her fellow first-years and cheered on regular classwide pingpong tournaments in the UNTHSC student lounge prior to the pandemic.
During Fort Worth’s safer-at-home directive, she spent the majority of her time alone in her apartment.

Jonas Kruse meets his classmates via Zoom during the COVID-19 stay-at-home order. Photos by Joyce Marshall
“It was never in my plan for med school to study at home,” said Kinard, who wondered at points if she should return to Chicago, where her mother lives.
Virtual Learning
Rather than relying solely on textbooks, the school’s students are expected to pursue their own research to uncover answers and additional questions.
Shah, who is dyslexic, finds study groups and online videos helpful.
“The support of the school is next level if you’re willing to let it in,” he said.
Before the pandemic hit Texas, Shah and his fellow students frequently sent classwide texts to organize outings like an afternoon at a museum or dinner out.
In the wake of COVID-19, some students who had traveled home for spring break stayed put, heightening the sense of distance many felt.
Losefsky believed she might have fared well because she has a built-in study partner in housemate Shah. The two started off the academic year as strangers and clicked almost immediately. In December, Shah purchased a town house near the UNTHSC campus.

Though strangers just a handful of months earlier, medical student Quinn Losefsky and Dilan Shah became roommates. Photo by Mark Graham
Losefsky moved into one of his spare bedrooms right as the pandemic began to ravage Italy. A lifelong athlete, she spent weeks tweaking a routine that no longer included the gym, library and coffee shops.
“I’m always reevaluating what works for me,” she said. “I love med school and don’t ever want to burn out.”
Throughout the COVID-19 crisis, Shah said he was adapting well in part because he came into medical school with solid tools. The Austin College graduate practices Vipassana, a form of meditation that he describes as accepting one’s reality — angst, fear and all.
After meditating under his favorite tree near the Trinity River, Shah said he feels centered, focused and calm. As a would-be psychiatrist, his interest in the benefits of meditation could help shape his career.
Esparza, who shares an apartment with two classmates, felt a surge of angst upon learning in April that school would remain online-only through the remainder of his first year.
“I am going to have to be more outgoing on virtual chats,” said the aspiring oncologist. “The isolation is taking a toll on the connection we have.
“The school has done an excellent job of making the curriculum online,” he added, “but it’s hard to replace being face to face with everyone.”
From the desk she ordered online when libraries closed, Kinard joined classmates in courses such as Patient-Centered Inquiry Based Learning.
On Mondays, groups of seven or eight students would receive a patient case designed to promote realistic and inquiry-based learning and cooperation among classmates. By Friday, each group was expected to have the case solved.

Jonas Kruse talks with this Patient-Centered Inquiry Based Learning classmates. Kruse said the coronavirus pandemic changed the way his classmates communicate. Photo by Joyce Marshall
In late March, the students met virtually to consider a patient with Bell’s palsy, a sudden weakness or paralysis in facial muscles that often proves temporary. They researched symptoms and underlying causes to come up with interventions and recommendations for treatment.
“It’s working OK,” Kinard said, “but I’m finding myself less willing to be vulnerable and ask questions when we’re separated digitally.”
“The communication is not nearly as rich because we’re not together, and our group is definitely more quiet,” Kruse said. “But if this had to happen, I’m really grateful it was during our first year instead of later, when nearly everything is clinical.”
“There are things like seeing patients and physical exams on the standardized patients that we can’t do remotely,” Flynn said, “but none of that is career-altering or will even impact their residency placement.”
Finding Mentors
Online classes disrupted more than camaraderie. Esparza said he missed interactions with the faculty, which numbers nearly 450 physicians, scientists and public health practitioners.
“Whenever I start to think about how expensive the school is,” Shah said, “I look around and remind myself there are always at least five doctors near us.”
Most medical schools break students into small groups and have a new physician interact with them every week, Flynn said. At the TCU and UNTHSC School of Medicine, students will work both one-on-one and in small groups with some of the same MDs all four years.
“We don’t often say it this way,” Flynn said, “but physicians are teachers.”
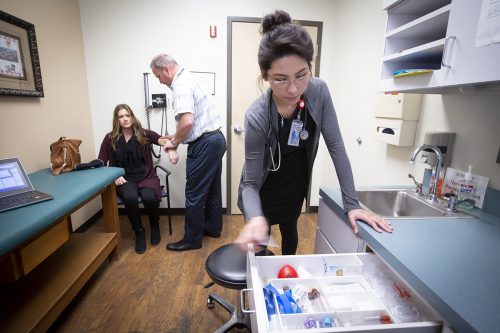
Before the coronavirus pandemic, Ive Mota Avila had Longitudinal Integrated Clerkship sessions with Dr. Shaun Kretzschmar twice a month in Aledo, Texas. The program gives students clinical experience early in their education. Photo by Joyce Marshall
When these students become residents or senior medical students, they will train those below them. Most medical students will spend a lifetime learning from senior colleagues and teaching junior colleagues.
The close ties with faculty translate into another layer of emotional support.
During the first week on the TCU campus, the students attended a pep rally where the faculty divided them into six teams. Ten new students will join the teams each successive year, and two physicians coach each group.
Physician-coach Dr. Debra Atkisson doubled down on her students’ well-being in the wake of the pandemic. The Fort Worth psychiatrist met weekly via Zoom with her team of 10 students, which includes Esparza, Losefsky and Kruse.
Atkisson often asked her students how they were maintaining a sense of normalcy during such an abnormal time.
“One of the things the school has done such an amazing job at,” she said, “is working with students on their own awareness of compassion, empathy and whole-person view.”

Dilan Shah and Quinn Losefsky wore sewn-together holiday sweaters to welcome students to the School of Medicine Winterfest, an event to help socially support the medical students. Photo by Mark Graham
During the first six months of the academic year, Atkisson saw the students at frequent social events, such as a Friendsgiving dinner at Joe T. Garcia’s and the student-initiated Winterfest. Shah emceed the holiday gathering, which featured student vocal performances, a baking contest and a gift exchange.
Esparza became particularly close to Atkisson (“She can crack me like an egg!”). He sought her out in early February to discuss what he saw as a growing problem with focus.
“I wait for the anxiety and the thrill of test week to come around,” he said, “and I don’t want to rely on that anymore.”
Empiric Education
Shuttered, too, as a result of COVID-19 were the students’ clinical rotations, a big draw for many. Kinard gave up a spot at Dartmouth University’s medical school when she was pulled off the waitlist at the TCU and UNTHSC School of Medicine.
She and the rest of her classmates gambled on an institution with neither a reputation nor a track record in large part because of its intention to approach medical school differently.
“From the outset,” Kinard said, “they pushed us to be vocal by giving us so many opportunities to communicate with the school and with each other.”
Most medical students in the U.S. spend hours a day attending traditional lectures, particularly during their first year. None of the classes at this medical school are in a lecture format.
Another hallmark of the school is that every student works with patients under the supervision of physicians throughout their four years. Some medical schools, including those at Harvard and Duke universities, offer similar training, but their programs do not begin until year three, and not every student participates.
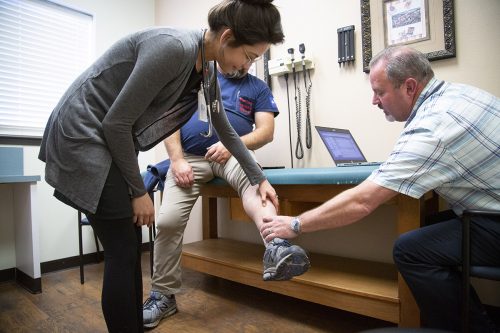
Ive Mota Avila examines patient Russell Webb with Dr. Shaun Kretzschmar. MD students have the opportunity to see the same patient through the course of care. Photo by Joyce Marshall
Avila was assigned to do an integrated clerkship at the Aledo Family Medicine Clinic in Aledo, Texas. Thirteen days into 2020, Russell Webb visited the clinic. He told Avila, who stood in an exam room beside Dr. Shaun Kretzschmar, that he was not doing well.
With an upward tilt of his chin and a note of outrage in his voice, Webb announced that he had gained weight between Thanksgiving and Christmas — far more than the stereotypical 5 pounds. Fifty, maybe 60 pounds, he conceded.
Avila asked if Webb were taking any new medications or supplements. No, and the arthritis in both shoulders and his numb fingertips weren’t getting any better.
Would he consider a steroid injection, she asked, meeting his gaze.
“I’d rather be shot with a 9 millimeter than be shot with a needle,” he fired back.
Outside the exam room, Kretzschmar, a family medicine specialist, told Avila that she had done well with a patient who can be prickly.
“I like him,” said Avila, who first met Webb in the fall.
On that wintry January day, Webb was the sixth patient the doctor and student would see together in an hour and a half.
“Doctors need to walk in and develop trust with a patient in just a few minutes,” Charles Taylor, provost and executive vice president for UNTHSC, told the entering class in July 2019. “This school was created to regain that emotional intelligence.”
Until the pandemic reached North Texas, Kruse, Esparza and Losefsky spent two afternoons a month at Mansfield Medical Associates, an internal medicine clinic about 20 miles southeast of TCU. The students shadow physicians there as part of their training.
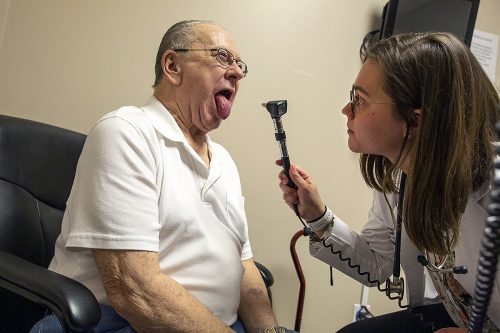
Quinn Losefsky examines Clifford Simmons at Mansfield Medical Associates in Arlington, Texas. Though only months into medical school, she correctly diagnosed the patient. Photo by Mark Graham
Losefsky “has come up with things that I didn’t expect a first-year student to catch,” said Dr. Khuong Phan, who sees around 100 patients a week in his office.
When Losefsky entered the room of Wayne Simmons, he greeted her like a friend or, perhaps, granddaughter, considering their ages. She’d seen him the previous month, on the day before she turned 23.
Losefsky donned purple gloves to examine Simmons’ swollen legs and listen to his heart. She excused herself to go tell Phan that she thought Simmons was in atrial fibrillation, one of several types of arrhythmia. The physician confirmed her diagnosis.
After the novel coronavirus compelled the medical school to pause the clinical rotations, Losefsky asked Phan if he could send her patient charts to review. When not studying or taking long walks, she would pore over the cases, wishing she could be back in the exam room.
“The patient must be at the center of everything we do every day, which is easy to say and very difficult to execute,” said Dr. Mohanakrishnan Sathyamoorthy, a cardiologist who chairs the school’s department of internal medicine.
Sathyamoorthy praised this group of students as “being collaborative, kind-spirited and empathetic. My general impression of this first class is it’s a homerun.”
Living Laboratory
Not every patient the students saw during their first year suffered real symptoms. As part of their curriculum, students worked with standardized patients, professional actors who prepare and rehearse for hours to play their parts.
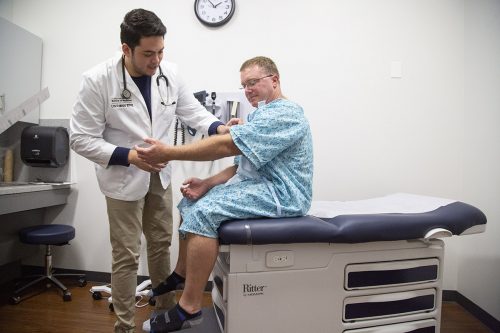
Edmundo Esparza examines standardized patient Chris Clark in a clinical skills session. Photo by Joyce Marshall
Four months before the students arrived on campus, Melinda Massie was one of 90 actors hired to perform a variety of patient roles on a rotating schedule. Her stage would be an examination table; her costume, a hospital gown.
Prior to every student encounter, Massie and the other standardized patients called for that week’s class attended a three- or four-hour training session where they received a dossier on the case.
Details of the individual they were set to portray included name; age; family life; medical, personal and family histories; education; diet; number of sexual partners; medicines; and allergies.
The actors also learned about the disease, disorder or condition that compelled their character to seek medical attention.
“We get down to extremely specific details like ‘I have two golden Labs named Duke and Paisley,’ ” Massie said. “And we are told about our personalities, if we are shy or outgoing, and how this particular patient would react to the students’ questions.”
The goal is for all of the students to have as close to the same experience as possible when they interview and examine their standardized patient, portrayed by a variety of actors.
On the UNTHSC campus, cameras are mounted in exam rooms so realistic they even have the antiseptic aroma of a typical doctor’s office.
Faculty members watch student-patient interactions from a control room. Also observing is Clare Shaffer, a theater director who oversees the actors in her role as the school’s clinical skills educator.
“Sometimes Clare would message me through an app saying I had a little more ‘natural sunshine’ than my colleagues, and I’d need to dampen that a bit,” Massie said.
Before stepping in the room, the students, who would later view video of their encounter, received a folder with the patient’s chief complaint and a nugget of information about the individual.
During the ensuing patient exams, students needed to ask questions in an organic way rather than sounding as though they were firing off bullet points or reading off a checklist or script.
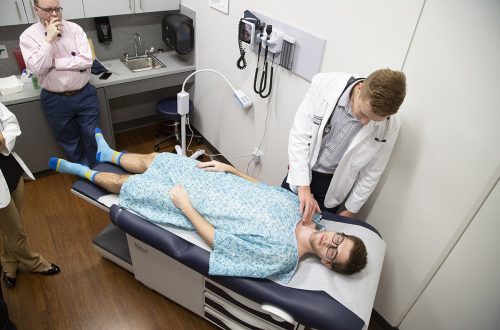
Faculty member Frank Sloan, left, observes as Jonas Kruse practices examining standardized patient Michael Carver-Simmons in the clinical skills lab. Photo by Joyce Marshall
After the transition to telemedicine in the spring — a step many physicians around the country took out of necessity — Massie missed the energy of being around the students. She also said she had to up her game when it came to looking for their nonverbal cues to critique.
A comment she might make to a student after the exam is that “they scrunched up their eyebrows” when Massie said, while in character, that she had an open marriage. “Something like that might make a patient feel judged.”
In December, Esparza was doing a routine cardiac exam on a standardized patient when he detected something through his stethoscope that didn’t sound right. Two doctors came and listened to the man’s chest, agreeing they picked up a faint murmur as well.
“It was a little scary,” Esparza said.
“If you’ve gone to a doctor and it doesn’t feel like the conversation is formulaic, it means the doctor is good at what they are doing,” Kruse said. “It’s not easy. I find that if a patient is more short with their answers, it gives me less time to formulate my next questions.”
Losefsky walked out of her first graded encounter and realized she had neglected to ask about suicidal thoughts.
“I figure it’s better to forget now,” she said, “than on a real patient.”
Renewed Dedication
As a young physician in the San Francisco area in the 1980s, Flynn treated patients early in the AIDS crisis when no one knew what caused the disease or how it spread.
Now, as health care workers around the country risk their lives in the fight against COVID-19, students including Losefsky, Kinard and Esparza said they had no qualms about their chosen profession.
Kruse, who was born in Germany and came to the U.S. at age 3, spent many childhood hours in the hospital with his father, who had a thriving geriatrics practice.
Even before the unit on neurology, Kruse gravitated to a future in acute neurological care, such as treating strokes and seizures.

Ive Mota Avila arranges her locker at the UNTHSC campus before her first year of medical school starts. Photo by Mark Graham
Avila has long wanted to work with women, inspired by her immigrant mother, who worked as a janitor and a restaurant cook to help make her daughter’s dreams come true.
Avila’s mother also never had a women’s health care provider with whom she could communicate in her native tongue.
“I want Spanish-speaking women to feel empowered to speak for themselves about their sexual health and reproductive options with another woman who understands both their language and culture,” Avila said. “Me.”
The pandemic gave Esparza time to think about his four-year research project. Unlike most U.S. medical schools, this one requires students to pursue a single line of research leading up to their degree.
Weeks into lockdown, Esparza finalized his project summary. He plans to identify the potential positive effects of exercise and neoadjuvant therapy (chemotherapy administered prior to surgery) on patients with gastrointestinal cancer.
By studying muscle strength, quality of life and other variables with patients who have completed chemotherapy, Esparza hopes to discover whether patients who both exercise and have the additional therapy rebound more quickly following treatment.
Crisis Response
As the pandemic widened, Esparza and many of the other students found themselves grappling with larger implications for their profession.
Losefsky resisted temptation to book a cheap flight to the beach in part because of the optics. Future physicians, she said, needed to be among the first to follow social distancing guidelines.

A nationwide blood donation shortage during the COVID-19 outbreak inspired students like Dilan Shah to donate. Still in the midst of classes, he took the opportunity to study on his phone. Photo by Mark Graham
She did answer the call in early May for a blood drive. Losefsky has O-negative blood, making her a universal donor.
Shah helped with a student-led effort to collect personal protective equipment for local physicians running out of masks, gloves and other essentials.
Kinard, Avila and classmate Kavneet Kaur collaborated on an effort to assist Samaritan House, which provides permanent housing and support for 60 residents living with HIV and AIDS.
Kinard also harnessed social media to help stop the spread of misinformation and to connect with physicians. She created a Twitter account to follow health care professionals and also patients tweeting during their isolation.
“It’s interesting to absorb the information and acknowledge the missteps,” she said, “so I’ll be prepared in three years not to make the same mistakes.”
Kruse devoted 72 hours to answering phones at Tarrant County’s COVID-19 hotline.
In a room by himself on the UNTHSC campus, he received upward of two dozen calls during a March shift. Kruse helped callers determine whether they should go to the hospital, seek a test for the virus or stay home and wait.
“As first-year medical students, we’re not really an asset in terms of workflow,” Kruse said, “but we’ve gotten a lot more clinical experiences than most other first-years.”
In May, he volunteered to trace coronavirus contacts by phone. “It doesn’t feel good to do nothing,” he said.
Sathyamoorthy said he considered the students’ combined efforts a source of pride. “These students who have a limited skill set in terms of health care delivery are still human beings who want to do their part.”
Moving Up
As the students wrapped up their first year of medical school, they had acquired a baseline in clinical sciences, including a foundational understanding of major organs and body systems.

Dilan Shah studies in one of the smaller breakout rooms on the third floor of the UNTHSC building that houses much of new medical school. Photo by Mark Graham
They had learned about anatomy, mental illness and life cycles using everything from high-tech simulations to handwritten flash cards. They know their way around a stethoscope, a skill that can take years to master.
“They also understand disease and death about 10 years earlier than their peers,” said Flynn, echoing something he was told during his own days as a medical student.
“Very quickly you realize this is not a TV show,” he said. “You develop both a respect and fear for diseases and death.”
Looking back on a year that defied expectations, the students seemed united in their excitement about the future. Year two will differ in that they will meet as a class only once a week.
Come September — so long as COVID-19 does not further disrupt plans — the students will spend the majority of their time in clinical rotations.
“This past year went so much faster than I expected,” Losefsky said. “But whenever I missed the group, I’d remind myself that these people are going to be my colleagues forever.”

Jonas Kruse attended his classes at home with his dog Harley on Monday, March 16, 2020, the first day of remote classes since the COVID-19 outbreak. Photo by Joyce Marshall
The year also flew by for Kruse who in April bought a house in Fort Worth with his wife, Anabel, whom he met as an undergraduate at Baylor University.
During the white coat ceremony at the start of the academic year, Kruse drew laughs with a remark that he and his fellow students “were about to become physicians in a short seven to 10 years.”
In recent months, a gravitas has settled on him, particularly given the speed of his first year of medical school, along with its twists and turns.
“I keep telling myself that if I can do this, I can do the next level,” he said.
“One step at a time.”

Your comments are welcome
1 Comment
I’m endlessly fascinated reading about medical issues and especially enjoyed the glimpses into these future doctors’ experiences. When I graduated from SMU in 1965, women didn’t become physicians. If I had my life to do over again, I’d definitely think seriously about being a P.A!
Related reading:
Campus News: Alma Matters
Dr. Terence McCarthy Leads New Medical School’s Emergency Program
The doctor is the John M. Geesbreght MD, MS, FACEP Chair of Emergency Medicine — the first endowed chair position at the TCU and UNTHSC School of Medicine.
Campus News: Alma Matters, Research + Discovery
Hands-On Learning Helps Medical Students Put Patients First
TCU and UNTHSC School of Medicine’s Dr. Stephen Scott discusses the school’s integrated approach to education.
Features
Stuart D. Flynn, M.D., Dean of Fort Worth’s New Medical School
TCU Magazine Editor Norma Martin spoke with Flynn about the evolution of medical school education and the opportunity to develop an innovative M.D. school in the 21st century.