
Angel Sheu has helped expand access to the life-saving overdose reversal medication, naloxone, through her Scholarly Pursuit and Thesis project.
Tech to the Rescue
A simple QR code developed by a TCU medical student could cut opioid overdose deaths.
A half-dozen medical students stood around a simulated patient, examining its facial structure and counting its breaths.
As the manikin stopped breathing, Angel Sheu, a second-year medical student at the Anne Burnett Marion School of Medicine at Texas Christian University, opened a box of naloxone, more commonly known as Narcan, retrieved a nasal mister and inserted the medication into the manikin’s nostrils.
She squeezed a dose of the lifesaving medication, and the manikin began breathing again.
“The chance of hurting someone [with naloxone] is less than 1 percent, but the chance of you saving them is 90 to 100 percent,” said Dr. Ric Bonnell, an assistant professor at the Burnett School of Medicine. “We try to have it as the default for anybody that’s down and not breathing.”
Sheu did this under the watchful eyes of Bonnell and Callie Crow, a retired paramedic and founder of the nonprofit Drew’s 27 Chains, during a training session on how to use naloxone to reverse an opioid overdose.
This type of training isn’t routine for future physicians or first responders. Being prepared to use naloxone in a life-threatening situation is still considered specialized training that health care providers, or even the general public, have to seek out in the United States, reports the National Institute on Drug Abuse.
Providing this information to medical students as they embark on their journeys to become physicians is critical, Crow said. “Having a physician that is aware of this crisis — and the fact that anyone can help someone live and recover from this — is right up there with CPR. It’s a lifesaving tool.”
To reduce opioid overdoses, which are now the leading cause of death for Americans between ages 18 and 45, Crow, Bonnell and Sheu have come up with a new approach requiring only a smartphone. “It’s right there at their fingertips,” Sheu said.
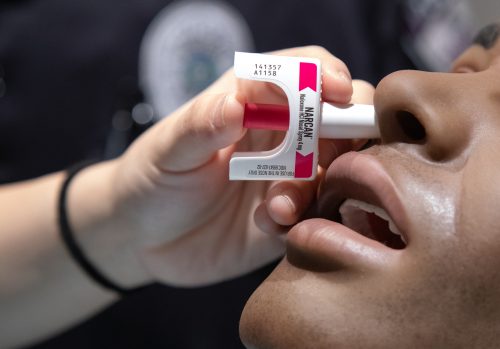
Training on how to use naloxone to reverse an opioid overdose is not standard in the United States, even for medical professionals.
Sheu is working on her four-year Scholarly Pursuit and Thesis student research project with Drew’s 27 Chains and Bonnell, her faculty research mentor. The Scholarly Pursuit and Thesis course is designed to push medical students to become lifelong learners capable of critical inquiry through research. Medical students tap into their curiosity and find evidence-based approaches for basic and clinical research.
Sheu put a creative twist on the naloxone distribution program by using existing technology to create a continuous loop of sharing information and distributing the lifesaving medicine. Anyone who receives free naloxone training from the nonprofit will also receive a free box of the drug with an accompanying QR code. Users can scan the QR code, quickly input data about a lifesaving event in which the dose was used and order a new dose for free.
“This data is going to be so important to take that next step into the education and awareness of opioid overdoses,” Crow said.
DIFFERENT PATHS, SAME PURPOSE
Crow has a vested — and spiritual — interest in preventing fatal opioid overdoses.
On June 12, 2020, during the height of the Covid-19 pandemic, her life changed forever. She was finishing a shift as a paramedic when she received a call that her son Drew Crow, 27, had been rushed to a hospital with fentanyl toxicity, more commonly known as a fentanyl overdose.
“As a parent,” Crow said, “that is the worst thing you could ever think of.”
The first responders hadn’t been trained to use naloxone, which was available at the time, but they got Drew to a North Texas hospital. A few hours later he died.
“I never imagined it would end like it did,” Crow said.
Shortly after her son’s death, Crow started Drew’s 27 Chains and found her purpose in life.
“It took me a long time to get there; it took me a long time to hear those words and not feel guilty,” Crow said. “But it was the only choice that I was left with.”

Drew’s 27 Chains trains people to use naloxone to save the lives of opioid users who overdose. The nonprofit has taught groups in Texas, Oklahoma and Antigua. Courtesy of Callie Crow
She began sharing her emergency medical expertise with other North Texans to help save lives. Since 2020, she’s trained more than 10,000 people and given out more than 10,000 free doses of naloxone in Texas, Oklahoma and Antigua. Many of the recipients have been first responders.
“Those are the people on the front lines, and those are my peers,” Crow said.
However, educating people about the importance of having naloxone and using it properly has been challenging because of the stigma associated with opioid use.
“A lot of people believe that people who are dependent upon opioids are homeless or they fit a particular type of demographic,” Crow said, “and that’s just not true.”
Opioids include fentanyl, oxycodone, hydrocodone, codeine, morphine, heroin and more. The drugs are often used as prescription medications to relax the body and relieve pain, but they can become addictive if misused. The use of opioids alone or in combination with other drugs is a major factor in overdoses in the United States.
To fight the stigma, Crow shares her son’s story during training sessions.
Drew Crow was 6-foot-4 with a fun-loving personality, an aspiring political journalist studying at the University of North Texas. He married Adriana Ogeda in November 2018 and enjoyed a happy marriage.
“A lot of people believe that people who are dependent upon opioids are homeless or they fit a particular type of demographic, and that’s just not true.”
Callie Crow
Outside of his decade-long battle with opioids, he was normal, Crow said. “Drew’s story is so powerful. People can relate to his story.”
In August 2023, her work caught the eye of the Office of National Drug Control Policy, and she was invited to the White House to share Drew’s story. So far, 74 of the more than 10,000 doses of naloxone she’s given out have been credited with saving lives.
“After that first notification … I was floored,” she said, “but then that just fueled it.”

Drew Crow was 27 when a fentanyl overdose killed him. Courtesy of Callie Crow
In her training, she emphasizes the age range of the people she’s helped save: from 13 to 89 years old. “It is such a wide variety of people,” she said, “and there is no demographic that is exempt from this.”
Sheu also saw the breadth of people affected by opioid overdoses long before stepping foot in medical school. As an undergraduate at the University of Denver, she became an emergency medical technician.
Three years later, she was a paramedic. For six years before she started medical school, she treated hundreds of people for opioid overdoses in Denver and Philadelphia.
“I’ve seen it in a variety of ways, from a simple opioid overdose and something more complex with a bunch of different drugs or alcohol,” Sheu said. “I see how it affects the community.”
That experience sparked an idea to raise awareness about opioid overdoses, educate the public on how to use naloxone and make the treatment accessible through technology. The idea didn’t become real until she met Crow at TCU. Sheu attended a naloxone training session that was part of the service-learning curriculum at the Burnett School of Medicine, where Bonnell introduced the two.
“It was kind of a perfect connection,” Sheu said. “We were able to collaborate and really foster this idea of Narcan training and then bring it to life.”
GETTING SOLID NUMBERS
Crow said that while she knows the effort is making a big impact, collecting accurate data on the number of lives saved has been difficult.
To count as a life saved, the responder must have attended a training session and used a dose of naloxone from Drew’s 27 Chains to reverse an opioid overdose. The person receiving the dose must test positive for opioid use after the incident and must survive. Obtaining critical data about the patient and the scenario is difficult without a simple mechanism in place to share information.
“There’s so much data that can be drawn from these situations that will help others in the future decide what the training needs to look like,” Crow said.
Sheu came up with the idea to equip each naloxone box with a simple-to-use QR code to better track results. “I’m absolutely sure that we’re saving more lives than are reported,” she said.
To quantify the impact, researchers must ask specific questions: How old is the patient? Where did the incident occur? Was naloxone readily available? Who had it? Where was it kept? How long did it take to administer the dose? What was the response to naloxone being administered? Was the person responsive by the time the paramedics arrived? And, ultimately, what was the result of the incident?
By scanning the QR code, the user can easily input the data and order another lifesaving dose from the nonprofit.
“Being able to get solid numbers,” Sheu said, “we could turn it into better training, see how we can improve and see the impact we’re making on the community.”

Angel Sheu, center, uses a medical manikin to demonstrate to TCU police officers Donald Nolty, left, and Tom McLaughlin how to administer naloxone nasal spray.
This type of data research is different from the work in a scientific lab that is a hallmark of traditional academic medicine. Still, this work can impact a community, said Michael Bernas, associate professor of medical education and director of Scholarly Pursuit and Thesis at the Burnett School of Medicine.
QR code technology “is common, and it’s so easy to do,” Bernas said. “The younger generations live on their phones, and they know exactly what to do with them.”
Sending replenishment doses to people who share data is a huge win for the nonprofit fighting to reduce opioid deaths. People are more likely to feel empowered that they can save someone’s life in a critical situation, Crow said. “Not because of some magical thing that happened, but because they are aware.”
Crow said she is confident the robust data will prove the efforts are making a bigger impact than she or Drew could have imagined. “It just creates so much positive that overcomes this negative, and I truly believe that we will win this fight of the opioid crisis.”

Your comments are welcome
Comments
Related reading:
Research + Discovery
Advancing Medicine
The Scholarly Pursuit and Thesis program gives students a competitive edge.
Research + Discovery
Deeper Compassion
Joe Hoyle’s capstone project examines the impact of empathy training on scuba volunteers.
Features
Med Students on a Mission
Three future doctors are serving the community through their own initiatives.